Anemia Drug Offers First-Ever Treatment For Illness Related To Inflammation
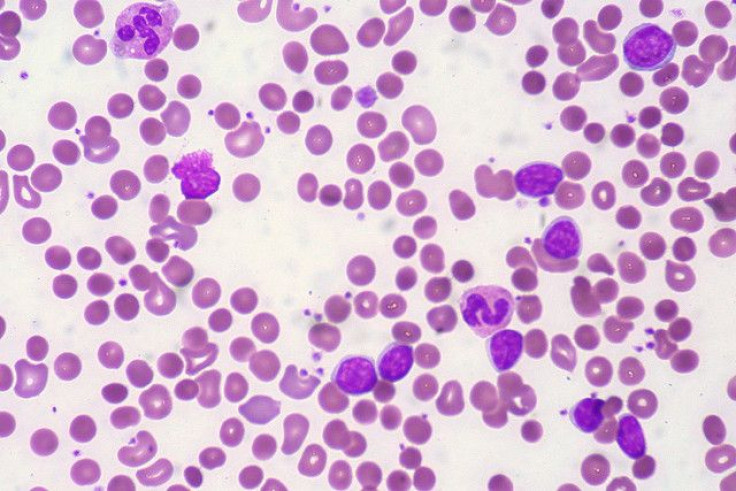
An experimental drug known as lexaptepid has shown early success at reducing inflammation and protecting iron levels in the blood of people diagnosed with anemia, a new study reports.
The form of anemia — a deficiency in red blood cell count or function, more generally — arises most often in hospitals. Known as anemia of inflammation, the condition occurs when patients’ immune responses kick into high-gear and trigger the secretion of a hormone called hepcidin. This hormone reduces the available supply of iron in the bloodstream, sometimes leading to anemia. Lexaptepid works by blocking hepcidin activation.
"It is quite encouraging that lexaptepid helped maintain appropriate levels of iron in the bloodstream of healthy volunteers without compromising the immune response," said lead study author Dr. Lucas van Eijk, of Radboud University Medical Center in the Netherlands, in a statement.
Anemia of inflammation differs from traditional anemia because it co-occurs among people with chronic illnesses. The Centers for Disease Control and Prevention estimates there are more than 130 million Americans living with a chronic illness. Understanding how these illnesses develop into related conditions, and how to treat them, stands as one of the great challenges of the 21st century — due in large part to the United States’s growing immunity problem.
With current treatment options, doctors are limited to targeting the underlying infection or illness, hoping to reduce inflammation by fixing the root condition. This approach, while ideal, is highly impractical. If doctors had the means to end a viral infection or a bacterial disease, patients would seldom stay in the hospital long enough to develop anemia in the first place.
Lexaptepid is an intermediary. Van Eijk and his colleagues tested the drug on 24 healthy male adults who were randomized either to receive the drug or a placebo. All volunteers received a low dose of Escherichia coli (E. coli) endotoxin to induce controled inflammation. Thirty minutes later, they received their treatment.
After nine hours had passed, the team checked back in to see how the subjects' iron levels were faring. Good news came for lexaptepid, which kept the levels as steady as they were before the dose of E. coli. The placebo, meanwhile, did nothing; iron levels continued to drop.
In addition, the team sought to test lexaptepid’s effect on the body’s immune response. Before testing, they’d hoped the drug would be able to inactivate hepcidin but keep the overall response intact. Their hypothesis was confirmed. While hepcidin failed to exhibit its normal iron-draining effect, all subjects still experienced similar flu-like symptoms: increased body temperature and white blood cell count, and higher concentrations of inflammatory and signaling proteins.
These were seen as positives because the human body still needs its immune system to fight off the major infectious agent, even if that means it’s weaker in other aspects. Increased body temperature and higher white blood cell counts mean the immune system is up and running. Van Eijk said the next step for anemia of inflammation research should involve delving deeper into lexaptepid’s effect on hepcidin.
"We are hopeful,” he said, “that, with further study, this first-of-its-kind therapy could significantly improve quality of life for patients suffering from chronic illnesses."
Source: van Eijk L, John A, Schwoebel F, et al. Effect of the anti-hepcidin Spiegelmer® lexaptepid on inflammation-induced decrease in serum iron in humans. blood. 2014.



























