Breast Cancer Deaths More Likely In Younger Women; Regular Mammograms Should Begin Before Age 50
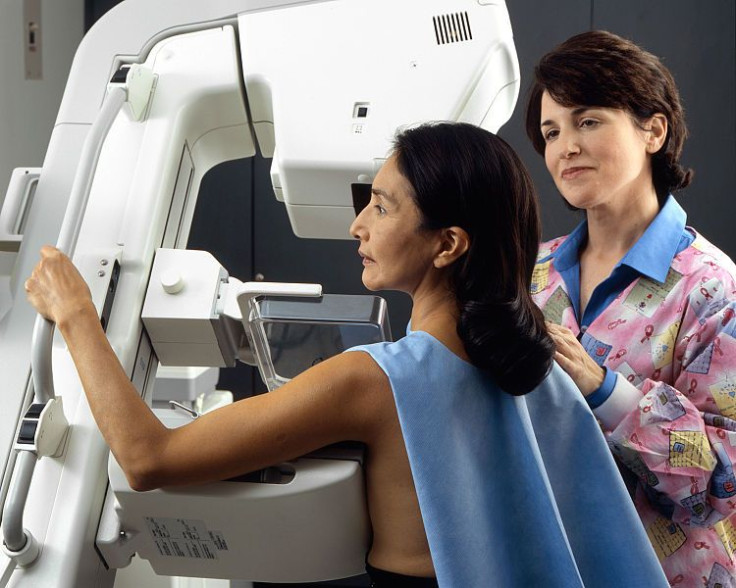
National estimates suggest that just under 40,000 women will die from breast cancer in the U.S. during 2013, while a little more than 232,000 new cases of invasive breast cancer will be diagnosed. Hypothesizing that breast cancer deaths mainly occur among women who have not undergone screening for the disease, researchers of a recent study published this month in Cancer discover that they are correct. Despite any certainty that these Boston researchers may feel, in all likelihood, they will encounter heated debate on the matter.
What Age?
Over the past few years, mammogram screening has become a point of contention despite the long-abiding American Cancer Society (ACS) guideline that “women age 40 and older should have a screening mammogram every year and should continue to do so for as long as they are in good health.” ACS also recommends that women younger than 40 have a clinical breast exam as part of a regular health exam at least every three years.
Yet, in 2009, the U.S. Preventive Services Task Force (USPSTF) made an announcement that raised plenty of hackles. Not only did USPSTF recommend a later age for mammogram screening — women between the ages of 50 and 74 — but this independent, volunteer panel of national experts also suggested that a mammogram be performed every other year instead of once a year. Many scientists in the field of cancer and women’s health immediately took exception. And then in 2011, researchers from the University of Colorado-Denver who studied potential benefits and harms of mammography came to an opposite conclusion. These researchers discovered that the “evidence made available to the USPSTF strongly supports the mortality benefit of annual screening mammography beginning at age 40 years, whereas potential harms of screening with this regimen are minor.”
Now, researchers once again look at this question, though this time they approach from a different angle.
Controversy Ended?
To determine whether early screening provides added benefits to women, researchers, including Dr. Blake Cady of Harvard Medical School and Massachusetts General Hospital, retrospectively evaluated mammography records for 609 breast cancer deaths. Other data examined during this study included surgical and pathology reports, recurrence and death dates, and demographics. The researchers found that, among the women who died of breast cancer, 29 percent were women who had been screened, whereas 71 percent were unscreened women — in particular, women who were never screened (65 percent).
“Most deaths from breast cancer occur in unscreened women,” the researchers wrote in their online article. “To maximize mortality reduction and life-years gained, initiation of regular screening before age 50 years should be encouraged.”
Interestingly, of those women diagnosed with fatal cancers, the median age was just 49 years. Because tumors in older women generally grow more slowly than those in younger women, the researchers noted that screening is more important for younger women.
“I did my medical training in the '60s, and I have seen with my own eyes the dramatic difference in mortality rates since breast cancer screening was introduced,” Cady told AuntMinnie.com.
Sources: Webb ML, Cady B, Michaelson JS, et al. A failure analysis of invasive breast cancer. Cancer. 2013.
Hendrick RE, Helvie MA. United States Preventive Services Task Force screening mammography recommendations: science ignored. American Journal of Roentology. 2011.



























