Colon Screening Participation Increases with Test Choice
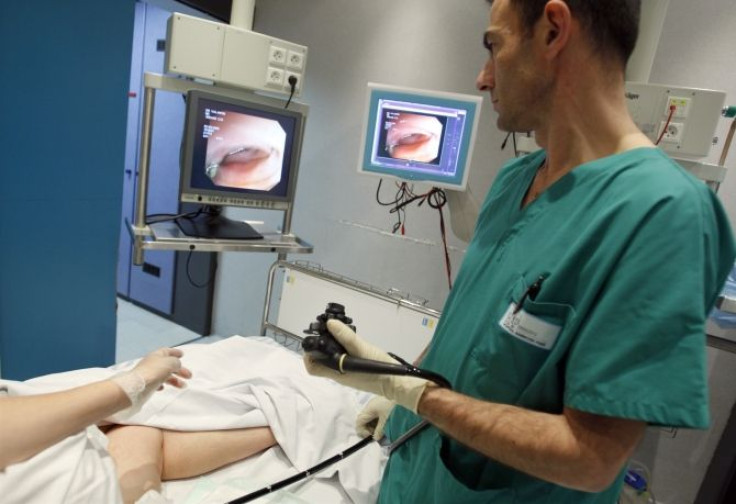
Colon screening participation increases when people are given choice between a stool test and colonoscopy or when the doctors recommend stool test instead of colonoscopy, study says.
Colorectal cancer or colon cancer is one of the leading causes of cancer-related death in US. Despite the fact that this cancer can be cured if detected early, not many people opt for regular colon screening. The Centers for Disease Control and Prevention (CDC) recommends that colon-screening must be done soon after turning 50. There is no single cause of cancer. Almost all colon cancers begin with benign ‘polyps’ that develop into cancer.
The research team that conducted the study on ‘Adherence to Colorectal Cancer Screening’ said that patients’ preferences should be considered when making colon screening recommendations.
The study led by John Inadomi of University of Washington School of Medicine in Seattle covered total of 997 patients who were divided into three groups.
In the first group patients were recommended to undergo colonoscopy by their doctor. Colonoscopy is a kind of screening test where the rectum and the entire colon are examined using a colonoscope. The advantage of this test being that the doctor can view the rectum and the entire colon. The doctor has an additional scope of removing any abnormal tissue for further testing. This is the most sensitive test available today.
In the second group, the participants were asked to undergo a stool test. In this test a sample of stool is taken and checked for any traces of blood.
The participants in the third group were given a choice between the two tests.
Overall, 58% of the participants underwent screening in a test of their choice or of their doctor’s.
The incidence of participants in the first group was as low as 38% when compared to 67% of participants who underwent the stool test.
When given a choice, 69% of the participants completed the screening test.
The study also found that attitudes toward screening-tests varied with ethnicity. Latinos and Asians completed screening more often than African Americans. Non-white participants preferred stool tests whereas white adhered to colonoscopy.
The study concludes that recommending a universal procedure to all patients might not be very helpful in getting compliance in screening tests for colon cancer.
“I would make sure that i took into account the patient’s preferences. I would flat out describe these tests... i think this goes against what a lot of us are doing right now. We should be finding out what patients prefer and really pursuing that”, said Inadomi to Reuters.
The study was published in the Archives of Internal Medicine.



























