Schizophrenia Drugs That Can Kill Antibiotic-Resistant Bacteria
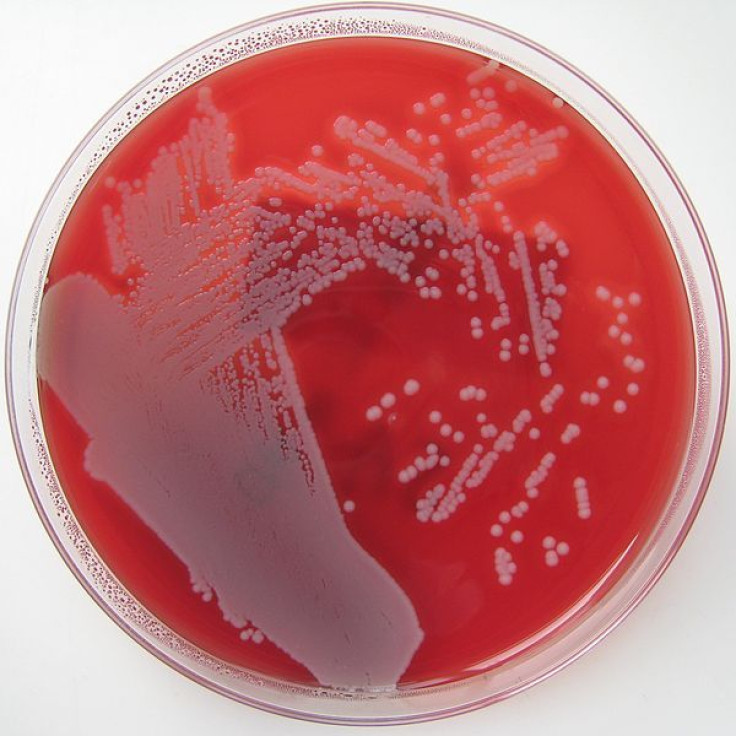
Although scientists have known for some time that thioridazine can kill antibiotic-resistant bacteria such as Staphylococcus aureus, they have never understood the mechanism by which it does so.
Until now. A new study from researchers at the University of Southern Denmark reveals why and how thioridazine, a drug formerly prescribed to treat the symptoms of schizophrenia, can work against antibiotic-resistant bacteria.
Global Issue
Antibiotic resistance is the ability of a microorganism to withstand the effects of an antibiotic. It evolves via natural selection through random mutation. The antibiotic action is an environmental pressure; those bacteria that have a mutation allowing them to survive will live on to reproduce. These bacteria will then pass on this trait to their offspring, which will be a fully resistant generation. Several studies have demonstrated that patterns of antibiotic usage greatly affect the number of resistant organisms that develop.
Antibiotic-resistant bacteria is a problem worldwide. Although Staphylococcus is often harmless, it is a common cause of skin infections, respiratory disease, and food poisoning. In 2008, researchers from the University of Southern Denmark proved that thioridazine could be used as a weapon against antibiotic-resistant bacteria, including Staphylococcus.
Now the same core research group, which includes Janne Kudsk Klitgaard, Hans Jørn Kolmos, and Birgitte H. Kallipolitis from the University of Southern Denmark and the Institute of Clinical Medicine, has tested thioridazine on Staphylococcal bacteria and discovered the drug works by weakening the bacterial cell wall. Ultimately, the interaction between thioridazine and antibiotics is what kills the bacteria.
"When we treat the bacteria with antibiotics alone, nothing happens — the bacteria are not even affected. But when we add both thioridazine and antibiotics, something happens: thioridazine weakens the bacterial cell wall by removing glycine (an amino acid) from the cell wall. In the absence of glycine, the antibiotics can attack the weakened cell wall and kill staphylococcus bacteria," explained Klitgaard.
New Purpose
The researchers said they will concentrate on finding ways to enhance thioridazine's ability to weaken Staphylococcal cell walls. Having conducted tests with the drug on roundworms, Klitgaard and her colleagues will next test the drug on mice and pigs. According to her, researchers are a little closer to a safe, nonpsychopharmacological drug that will save people from potentially fatal infections that do not respond to antibiotics.
Overuse of broad-spectrum antibiotics, such as second- and third-generation cephalosporins, has greatly hastened the development of antibiotic resistance. Other factors contributing to resistance include incorrect diagnosis, unnecessary prescriptions, improper use of antibiotics by patients, and the use of antibiotics as livestock food additives for growth promotion. Antibiotic resistant Staphylococcus is one of the five most common causes of infections after injury or surgery. For people who are immunocompromised or immunodeficient, this bacteria may be life threatening; it affects around 500,000 patients in American hospitals annually.
"Now that we know how thioridazine works, we can develop drugs that target the resistant bacteria. We can remove or inactivate the parts of thioridazine, which treats schizophrenia, so we end up with a brand new product that is no longer an antipsychotic," explained Klitgaard.
Thioridazine, an antipsychotic medication that works by changing the actions of chemicals in the brain, may still be available to patients who have failed to respond adequately to treatment with appropriate courses of other antipsychotic drugs, either because of insufficient effectiveness or the inability to achieve an effective dose. Thioridazine was found to trigger a serious type of irregular heartbeat that in rare cases could cause death.
"This will no longer be an antipsychotic, when scientists are finished with this task," Klitgaard said.
Many drugs arrive at their ultimate purpose only after being used for an entirely different reason. Propecia, for instance, was originally marketed as Proscar and was intended to treat the benign enlargement of the prostate. After five years on the market, it became known that one of the side effects of Proscar was hair growth on bald men; now it is used to treat male-pattern baldness. The well-known treatment for penile dysfunction, Viagra (or Sildenafil as it's officially known), was originally conceived as a treatment for hypertension, angina, and other symptoms of heart disease.
Source: Klitgaard JK, Kolmos HJ, Kallipolitis BH, et al. Thioridazine induces major changes in global gene expression and cell wall composition in methicillin-resistant Staphylococcus aureus. PLOS ONE. 2013.



























