Spinal Cord Double Whammy: Two Spine Surgeons Are 3 Times Safer (And Actually Cheaper) Than Just 1
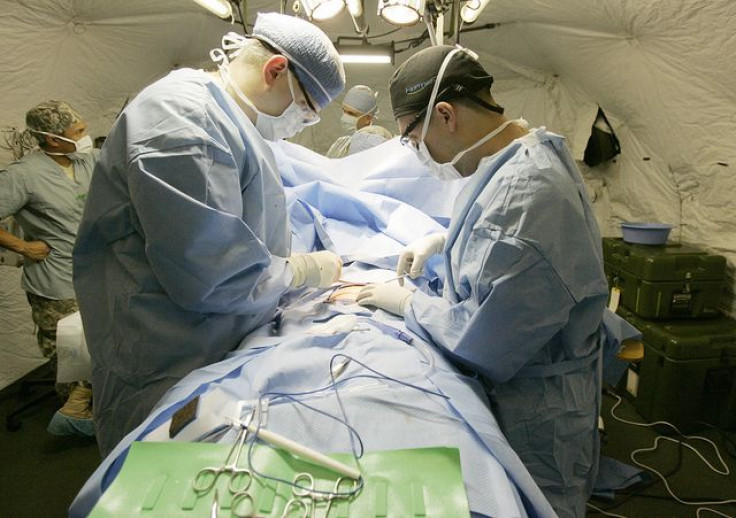
You don’t often think of spinal surgery when people say “The more the merrier,” but a new University of Washington study suggests maybe you should. Researchers found that a tag-team approach to spine surgery, in which a neurosurgeon and an orthopedic surgeon work together, yields the safest and most cost-effective results.
Reconstructive surgeries for conditions like scoliosis and kyphosis are long and difficult. They require a great deal of the surgeon’s energy, not to mention time, which leaves ample room for sloppy mistakes. Not only do they have to correct specific curvatures; they must avoid blood loss and a bevy of post-surgery complications. As of yet, there is no standardized protocol for spinal surgeries.
Researchers found that by coupling the skill sets of a neurosurgeon and an orthopedic surgeon, in addition to supporting the procedure with a live preoperative screening conference and monitoring blood loss throughout the surgery, patients enjoyed two-thirds fewer complications. Their study included 164 consecutive patients: 40 before and 124 after the new approach was implemented. In reviewing the success rate, the team found a dual approach most often avoided wound infection, deep vein thrombosis, pulmonary embolism, and urinary tract infections.
"We can shorten the operation when we have two surgeons in the operating room as equal partners,” said lead author and orthopedic spinal surgeon at Group Health Physicians, Dr. Rajiv Sethi, in a statement. The advance is especially poignant, he added, given spinal surgery “is among the most dangerous and complication-ridden of all operations.”
Basically, the protocol Sethi and his colleagues propose comes in three parts. The first is a meeting between multiple clinicians, including an internist, a physical medicine and rehabilitation physician, nurses involved with post-operative care, and at least two members of the anesthesiology team assigned to the surgery. The goal is to air out any unknown factors about the patient and determine through direct communication whether surgery is even necessary.
The other two components involve constant monitoring to make sure the patient doesn’t lose too much blood and a separation of responsibilities among the surgeons, who each has distinct duties related to their unique skill sets.
"Our findings could help medical teams at Group Health and around the country reduce complications—and likely cut costs too—while improving performance and patient outcomes," Sethi said.
However, he conceded that not all facilities may be equipped to handle two surgeons operating at once. For one thing, the doctors at Group Health and Virginia Mason, one of the hospitals used in the study, are paid on salary. Whether they perform half a surgery or an entire one is irrelevant. Not all doctors have this luxury, Sethi points out. “At medical centers where doctors are paid on a fee-for-service basis, with more pay for doing more procedures, it might be harder to institute this kind of systems approach, because it entails up-front costs and commitment from leadership."
Overall, the hope in conducting this research is to motivate facilities away from a model of doctor compensation and move instead toward patient satisfaction. Spinal fusion surgeries generally last several hours. Anything that can minimize the damage done in that time is probably worthwhile.
Source: Sethi R, Pong R, Leveque JC, et al. The Seattle Spine Team Approach to Adult Deformity Surgery: A Systems-Based Approach to Perioperative Care and Subsequent Reduction in Perioperative Complication Rates. Spine Deformity. 2014.



























