Closer To Treatment For Deadly Disease Tuberculosis: Scientists Discover Biomarker
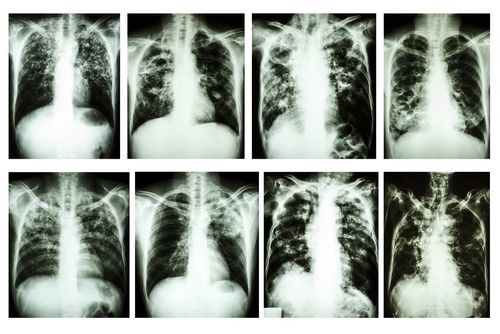
Scientists have found a key protein that can protect people from the highly contagious and life-threatening lung disease tuberculosis, leading medicine closer to finding new treatment strategies, which may be in the form of a vitamin D supplement. Researchers from Harvard University School of Public Health and the University of Michigan School of Medicine published their findings in the journal Science Translational Medicine.
After sorting through and analyzing genes from hundreds of tuberculosis patients in four different countries, the people who were diagnosed with the disease had higher levels of the newly discovered protein interleukin-32, which will help doctors identify people who are at the greatest risk for tuberculosis.
"Until now, there had been no way to predict, based on biological factors, why latently infected individuals do not develop active tuberculosis," the study’s lead author Dennis Montoya, a postdoctoral scholar in the division of dermatology at the David Geffen School of Medicine at UCLA, said in a press release. "We were surprised to find many differences between people with latent TB and healthy people, suggesting that people with latent TB may have activated immune systems that are protecting them from developing active infection."
A biomarker, which is used for researchers to spot a disease or infection such as tuberculosis, is necessary to explore different treatment routes, and IL-32 will serve as a new screening device for doctors. In the researchers’ experiments, IL-32 was able to stimulate the immune system and ultimately make it kill tuberculosis-causing bacteria. The catch is IL-32 only worked when the body had enough vitamin D, and low levels had already been known to put patients at higher risk for tuberculosis.
"When vitamin D levels were low, IL-32 was not able to kill the bacteria," the study’s co-author Dr. Robert Modlin, the Klein Professor of Dermatology at UCLA, said in a press release. "However, if we simulated the effect of supplementing individuals by adding vitamin D to the culture of the activated immune cells that had low vitamin D levels, IL-32 regained its ability to kill. Our findings suggest that raising standards for daily intake of vitamin D could help to protect against a TB pandemic."
Approximately one-third of the world is infected with tuberculosis, which attacks the lungs at first but without treatment can move onto the kidney, spine, and brain, and eventually become fatal, according to the Centers for Disease Control and Prevention. It spreads in the air between two people, most commonly through coughs, sneezes, speaking, singing, or any other way a person uses their lung capacity to interact.
A recent study published in the journal Nature found, after analyzing DNA from 1,000-year-old mummies, tuberculosis had spread a completely different way than they currently knew and that it actually originated less than 6,000 years ago in Africa. When tuberculosis goes into severe stages, the bacteria attacks the skeleton, which gave archaeologists clear signs to date the disease through centuries of family lineages. As one of the deadliest diseases on the planet, the new advents of discovering are helping scientists reconstruct history and their treatment approaches.
“This is a landmark paper that challenges our previous ideas about the origins of tuberculosis,” Terry Brown, a professor of biomolecular archaeology at the University of Manchester, told The New York Times. “At the moment, I’m still in the astonished stage over this.”
Researchers will continue to trace the historical roots of the disease, in addition to moving forward with new research to understand if vitamin D supplements can help prevent tuberculosis. Vitamin D is produced in the skin when exposed to the sun. However, dermatologists suggest taking an oral supplement rather than lying out in the sun for tuberculosis prevention.
"Our current strategy of antibiotic therapy, as well as methods of identifying which patients will develop severe disease, have remained essentially unchanged for decades," the study's co-author Barry Bloom, a professor of Public Health at Harvard University said in a press release. "Our findings of specific markers in the blood that can tell us which people are at risk can help countries focus limited resources on patients who have lower levels of this protein. In addition, this may point the way to new treatments for a disease that greatly needs them."
Source: Montoya D, Modlin R, Bloom B, Inkeles MS, Liu PT, Realegeno S, et al. IL-32 is a molecular marker of a host defense network in human tuberculosis. Science Translational Medicine. 2014.
Published by Medicaldaily.com



























