Insulin Pill Is Breakthrough In Diabetes Treatment, Provides New Way For Body To Lower Blood Glucose
Scientists have attempted to create a pill form of insulin treatment since the 1930s, so diabetes patients would be spared the pain of jabbing themselves with a needle every day. But in the past, such pills were deemed physically impossible — “left for dead because as a protein composed of amino acids, insulin is destroyed by enzymes in the digestive system before it can do any good,” Bill Berkrot of Reuters writes.
According to a new study published in the ACS journal Biomacromolecules, however, a team of researchers believe an insulin pill can be possible. They have found a new way to create a pill that digests properly in the stomach and is absorbed into the bloodstream, to lower the patient’s blood glucose, remove the pain of needles, and increase the likelihood that patients will take their medicine when they should.
Sanyog Jain, assistant professor at National Institute of Pharmaceutical Education and Research and a researcher who led the study, discovered two new approaches that would make it easier for an insulin pill to be absorbed properly into the body. Previously, scientists struggled with delivering insulin in a pill due to the stomach’s breaking down of insulin before it could get to work. Digestive enzymes break down the pill and prevent the insulin from being absorbed. Furthermore, it’s difficult for insulin to be absorbed through the stomach into the bloodstream. Jain found that when he packed insulin into small sacs made of lipids — known as liposomes — and layered them with protective polyelectrolytes, as well as folic acid, the insulin was prevented from breaking down in the digestive system. Folic acid is a type of vitamin B that allows liposomes to be absorbed into the blood through the intestines.
The scientists tested these “layersomes” in rats and found that this new system was able to decrease blood glucose levels nearly as much as injected insulin. However, they also found that the effects of the layersomes continued longer than that of injected insulin.
Diabetes is a disease that inhibits the production or use of insulin, which is a hormone that helps blood glucose — or blood sugar — become absorbed into cells and give them energy. Type 1 diabetes occurs when the body doesn’t make enough insulin, and type 2 diabetes occurs when the body doesn’t make or use insulin very well, causing glucose to remain in the blood, which can lead to serious problems.
Though an insulin pill would most likely be the most convenient treatment option, diabetes patients do not rely entirely on needles and syringes. There are currently other options available, including insulin pens, which inject a needle under the skin after the patient presses a button. External insulin pumps can be worn on a belt and can contain insulin for several days. Insulin is pumped into the body through tubes and a needle inserted under the skin, called a cannula. Injection ports are somewhat similar to insulin pumps, as a cannula is inserted into the skin, and it reduces the number of skin punctures from one a day to one every few days. Insulin can be injected through the port that is attached to the skin.
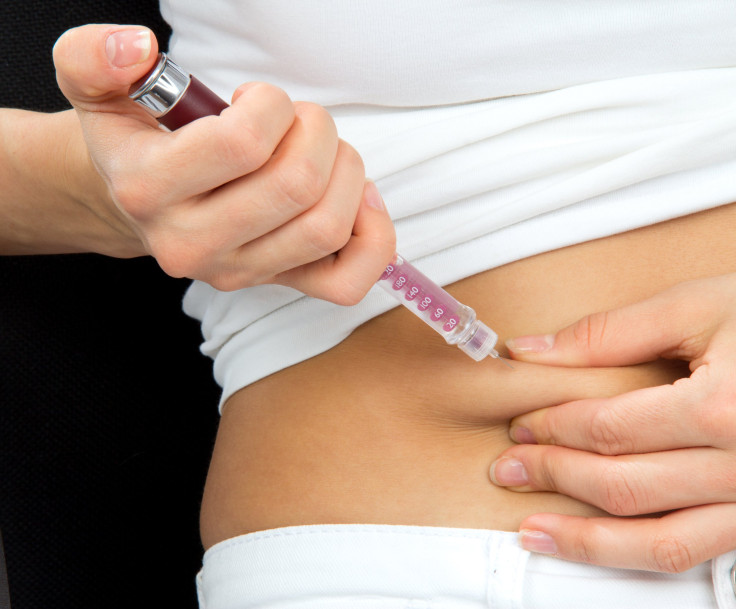
However, for all of the above treatments, punctured skin — and daily pain — is still required. So doctors and scientists have been trying to create an insulin pill, which would reduce the pains of inserting these needles every day.
Aside from the research published in Biomacromolecules, two other companies are currently vying to be the first to create the pill — a small Israeli company racing against a Danish pharmaceutical giant, what Reuters dubbed a “David and Goliath story.” Both Novo Nordisk, the largest insulin product company in the world, as well as Oramed Pharmaceuticals are hoping to develop a pill in the next decade. “We’ve built technologies and we’ve seen from studies in animals and early human trials that this may not be as impossible as decades of research had indicated previously,” Peter Kurtzhals, Novo’s head of diabetes research, told Reuters.
However, other health professionals are somewhat more cynical about the pill potential. “I’m not going to hold my breath on this one,” Dr. Robert Ratner, chief science and medical officer for the American Diabetes Association (ADA), told Reuters. “It would be an important contribution to the therapeutic armamentarium. But there are still great limitations in our ability to get the insulin absorbed and control how much insulin gets absorbed.”



























