Florida’s Pill Mill Laws Hope To Address State’s Opioid Epidemic By Cutting Down On Pain Medication Prescriptions
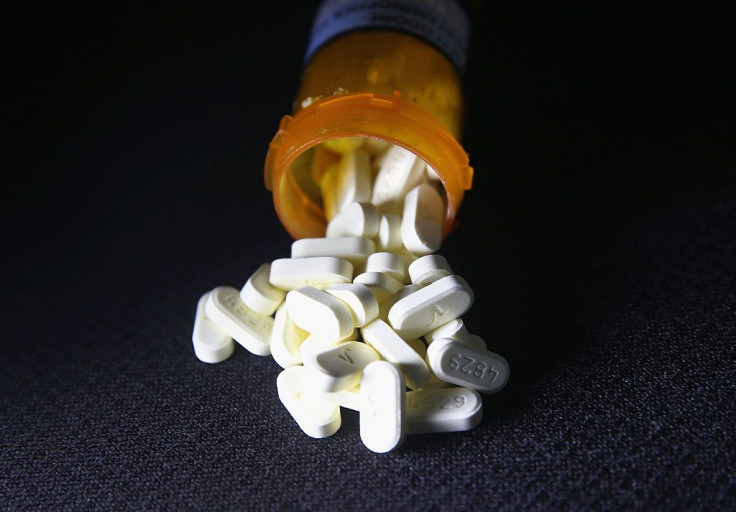
Opioid abuse and addiction has escalated severely in recent years, so policymakers got busy attempting to stem the flow of improperly and illegally prescribed painkillers. Florida was one state that took action, creating two laws meant to curb opioid prescriptions in late 2011. A group of researchers at the Johns Hopkins Bloomberg School of Public Health have analyzed the effects of these policies and found that, overall, the state’s top prescribers doled out significantly fewer doses of opioids following the laws’ implementation. Unfortunately, the laws did not change the behavior of a small group of providers that accounts for a disproportionately large number of prescriptions.
The analysis followed patients and prescribers between 2010 and 2012, both before and after Florida implemented its opioid policies. The first law created the Prescription Drug Monitoring Program (PDMP), which tracks prescription information including patient names, dates, and amounts of medication prescribed. That way, doctors can be aware of patients trying to get multiple prescriptions from different doctors — a behavior known to be associated with addiction.
The second law focused on pain clinics nicknamed pill mills because of their loose prescription policies. The new rule requires that such clinics register with the state and be run by a physician.
The researchers estimated that opioid prescriptions by Florida’s top prescribers fell by 6.2 percent during the year after the laws went into effect. That group provided 13.5 percent fewer prescriptions, and its number of patients also dropped by 5.1 percent. At the same time, the laws failed to slow the 4 percent of providers that accounted for a whopping 40 percent of the opioid prescriptions in the state. Primary care providers made up about half of the top prescribers.
“When we looked at the prescription numbers in the year before the two laws went into effect, we were very surprised at how concentrated the prescriptions were among a subset of prescribers,” said Dr. G. Caleb Alexander, the study’s senior author and an associate professor at the Bloomberg School, in a statement. “At the same time, these aren’t the only prescribers that we should worry about. There is an unmistakable correlation between the volume of opioids on the market and injuries and deaths from these drugs, and health care providers have a shared responsibility for the extent that these products are prescribed.”
The study’s results shed light on both the laws’ abilities and limits in curbing opioids.
“Our findings indicate how state policies such as PDMPs may reduce opioid use among the highest prescribers,” said Dr. Hsien-Yen Chang, an assistant scientist at the Bloomberg School and the study’s lead author. “But our report also shows that programs like PDMPs must be complemented by many other measures to combat the epidemic of addiction and nonmedical opioid use.”
The researchers note that it is difficult to separate the impact of the PDMP and the pill mill law, but say all doctors should check the state database before prescribing.
America’s opioid problem has reached epidemic proportions — an average of 44 people die of an overdose daily. In response to the issue, the Centers for Disease Control put out new guidelines for doctors detailing when they should be prescribing opioids. The center recommended that the drugs be given only when other methods of pain management have failed, and at lower doses and for shorter periods of time than in the past.
Dr. Alexander said he hopes checking the prescription database will become routine.
“I think we’ll get to that point; we’ll see prescription databases used like these other tools and have an even greater impact.”
Source: Chang H, Lyapustina T, Rutkow L, Daubresse M, Richey M, Faul M, et al. Impact of Prescription Drug Monitoring Programs and Pill Mill Laws on High-Risk Opioid Prescribers: A Comparative Interrupted Time Series Analysis. Drug and Alcohol Dependence. 2016.
Published by Medicaldaily.com



























