For Prostate Cancer, Surgery May Not Be More Effective Than Waiting
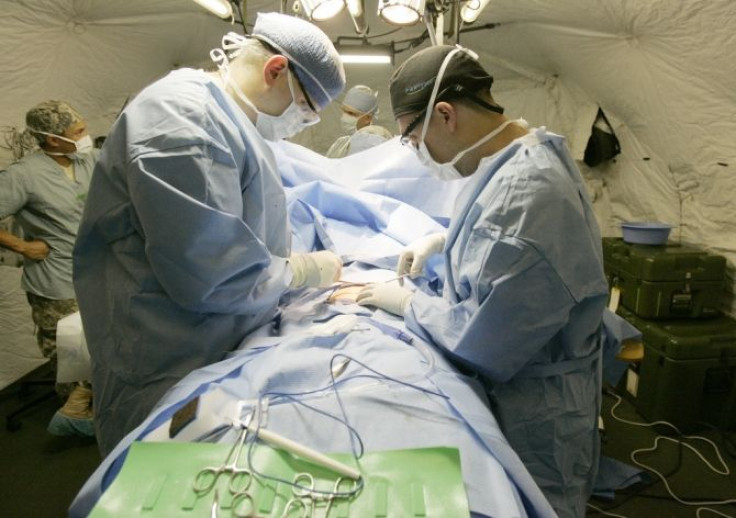
In fact, the researchers, led by Timothy Wilt, found that surgery did not cut the risk of death by a statistically significant margin, as compared to simple observation. Surgery created significant risks of side effects, such as incontinence and erectile dysfunction, while observation did pose an increased risk of the spread of cancer to the bones.
The study followed over 700 men over the course of a decade. For some, they were assigned surgery – a radical prostatectomy, where doctors remove the prostate and the surrounding tissue. The rest of the men were assigned observation. Of the men, 21 (5.8 percent) who were assigned a prostatectomy died; 31 (8.1 percent) who were assigned the wait-and-see approach did as well. Then, 10 years later, 47 percent of men who had chosen surgery had died; 49.9 percent of men who were observed had as well.
Some groups fared better than others. Men whose prostate-specific antigen, or PSA, score was closer to 10 seemed to require surgery much more than those whose scores were intermediate or lower. Men with intermediate- or high-risk tumors tended to fare better after surgery as well.
Many doctors remain unconvinced by the finding. As prostate cancer is usually a slow-growing cancer, 10 years may not have been enough time to find the true effects and differences between surgery and observation.
However, the study may perhaps be a ray of hope for men facing a prostate cancer diagnosis. Presently, about 10 percent of men choose the wait-and-see approach. Normally, experts say, when people hear the word ‘cancer,’ they want to do something aggressive to battle it. That may not be necessary.
Prostate cancer is the second-deadliest cancer for men, after skin cancer. It is said that most men, if they live long enough, will have a form of prostate cancer. But experts say that, despite its prevalence, most men are likely to die with prostate cancer, rather than from it.
The results of the trial's findings were published in The New England Journal of Medicine.



























