What Is Lyme Disease?: Signs And Symptoms Of The Invisible Illness
What disease, for which there is no vaccination, has increased nearly 25-fold since 1982 in its number of annually reported cases? What is the most common tick-borne illness in both North America and Europe?
Lyme disease.
According to recent research, in 2009 there were nearly 30,000 confirmed cases of Lyme disease. The Centers for Disease Control and Prevention (CDC) estimates that the real number of cases may be as high as 480,000. In 2011, 96 percent of Lyme disease cases were reported from 13 states: Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Vermont, Virginia, and Wisconsin. Cases have also appeared in Northern California and on the West Coast. It is important to note that the lone star tick, which is primarily found in the southeastern and eastern U.S., does not transmit Lyme disease.
History
In 1975, a cluster of children and adults residing in the area of Lyme, Conn. began to experience uncommon arthritic symptoms. By 1977, 51 cases of "Lyme arthritis," as it was referred to at the time, had been diagnosed, and a black-legged tick (Ixodes scapularis) had been linked to its transmission. Specialists attribute the emergence of Lyme disease in that part of Connecticut to man-made changes to the environment; previously farmed land had become reforested and then developed for suburban residential use, thus juxtaposing wildlife (and ticks) with people.
During 1982, Willy Burgdorfer discovered the bacterium responsible for the infection. Borrelia burgdorferi is a spirochete, related to the spirochete bacterium that causes syphilis. While an infected tick is drinking your blood, the bacteria are released into your blood stream. The corkscrew-shape of B. burgdorferi allows it to burrow and hide in your body's tissues, and this is why it causes such wide-ranging damage. It is now known that five subspecies of Borrelia burgdorferi exist, accounting for more than 100 strains in the U.S. and 300 worldwide, many of which may have developed some resistance to various antibiotics.
Serology testing became widely available in Connecticut during 1984. More than ten years later in 1997, the first Lyme disease vaccine became available. However, four years later, the manufacturer withdrew the vaccine from the market.
Transmission
Because some Lyme sufferers do not recall being bitten by a tick, some people, including Dr. Deitrich Klinghardt, believe the bacteria can also be spread by other insects, including mosquitoes, spiders, fleas, and mites. The CDC refutes this and also states that "there is no evidence that Lyme disease is transmitted from person-to-person. For example, a person cannot get infected from touching, kissing or having sex with a person who has Lyme disease." Congenital transmission, though, is less clear. "Lyme disease acquired during pregnancy may lead to infection of the placenta and possible stillbirth; however, no negative effects on the fetus have been found when the mother receives appropriate antibiotic treatment. There are no reports of Lyme disease transmission from breast milk," the CDC also says. Scientists have found that the bacteria causing Lyme disease can live in blood that is stored for donation, so individuals being treated for Lyme disease are advised against donating blood.
Although dogs and cats can get Lyme disease, there is no evidence that they may spread the disease to their owners.
Lyme disease is most often diagnosed based on symptoms and the possibility of exposure to infected ticks.
Diagnosis And Symptoms
As with blood tests for other infectious diseases, a serum test is expected to be negative during the first few weeks of infection. Several weeks after infection, the enzyme-linked immunosorbent assay (ELISA) test may detect antibodies to B. burgdorferi; if the ELISA test is positive, the Western blot is usually done to confirm the diagnosis. Accuracy of these tests and therefore diagnosis depends upon the stage of disease.
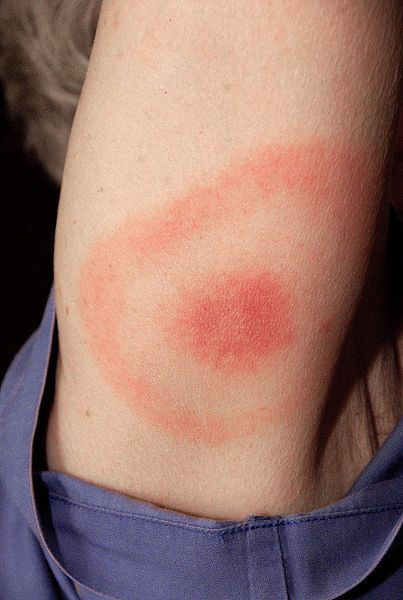
A small, red bump may appear at the site of the tick bite. Such a bump is normal after a tick bite and does not necessarily indicate Lyme disease. However, over the next few days, the redness may expand forming a rash in a bull's eye pattern, with a red outer ring surrounding a clear area. The rash, called erythema migrans, is known as a signature of Lyme disease yet for many people the rash may not appear as a bull's-eye. Some people develop this rash at more than one place on their bodies. Fever, chills, fatigue, body aches, and a headache — flu-like symptoms — may accompany the rash.
If left untreated, the infection can spread to joints, the heart, and the nervous system. At that time, symptoms may include joint pain and swelling. The knees are especially vulnerable, but the pain can shift from one joint to another. Within weeks, months, or even years after infection, a person may experience inflammation of the membranes surrounding the brain (meningitis), temporary paralysis of one side of the face (Bell's palsy), numbness or weakness in the limbs, and impaired muscle movement.
Several weeks after infection, some people develop these less common symptoms:
- Heart problems, such as an irregular heartbeat. Heart problems rarely last more than a few days or weeks
- Eye inflammation
- Liver inflammation
- Severe fatigue
Deceptions
The signature bull's eye rash is absent in nearly half of those infected and fewer than half of Lyme patients recall a tick bite, according to Dr. Joseph Mercola; in some studies, this number may be as low as 15 percent. Doctors refer to Lyme disease as "the great imitator," because it mimics other disorders, such as multiple sclerosis, fibromyalgia, chronic fatigue syndrome, and even Alzheimer's disease. Many patients with Lyme disease appear healthy and their blood work may even be normal. For this reason it has also been called the "invisible illness."
Treatment
Patients treated with antibiotics in the early stages of the infection usually recover rapidly and completely. Most patients who are treated in later stages of the disease also respond well to antibiotics, although some may have suffered long-term damage to the nervous system or joints. Approximately 10 to 20 percent of patients experience fatigue, muscle aches, sleep difficulty, or problems thinking — even after completing a recommended course of antibiotic treatment. These symptoms cannot be cured by longer courses of antibiotics, but doctors believe they generally improve on their own, over time.
According to Mayo Clinic, oral antibiotics are the standard treatment for early-stage Lyme disease. For adults and children older than eight, these usually include doxycycline; for adults, younger children, and pregnant or breast-feeding women, these usually include amoxicillin or cefuroxime. Intravenous antibiotics are recommended when the illness involves the central nervous system. This treatment is effective in eliminating infection, although it may take some time to recover from the symptoms.
With no vaccine currently available, prevention of Lyme disease includes using insect repellent and removing ticks promptly.
Source: Lyme Disease: A Public Information Guide. U.S. Department of Health and Human Services and Centers for Disease Control and Protection.
Published by Medicaldaily.com