Who Will Survive Surgery? New Model For Predicting Success Among Elderly Patients
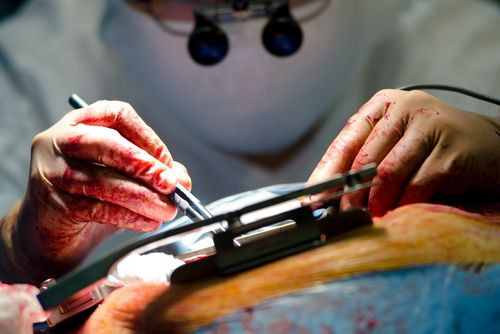
Over the past two decades, the geriatric population has increased dramatically, while the number of elderly patients who undergo surgery has concurrently spiked. Sometimes, when recommending surgery for their elderly patients, doctors fail to adequately factor fragility into the equation and this leads to unforeseen difficulties, and in some cases death. Now, a team of researchers has created a new multidimensional frailty score to help predict postoperative outcomes in older adults.
"This study was inspired by surgeon’s request," Dr. Kwang-il Kim, Seoul National University College of Medicine, wrote in an email to Medical Daily. "They were confused about predicting outcomes in older surgical patients, and they recognized there is something beyond the conventional tool (e.g. ASA class)." ASA class or American Society of Anesthesiology classification, then, was the status quo tool the researchers needed to beat when devising a new method. How did they fare? “We found that older surgical patients have surgical risks that can be predicted by careful review of their specific characteristics,” wrote the authors in conclusion of their published research appearing in JAMA Surgery.
Predicting Success for Geriatric Surgery
In the U.S., more than half of all operations are performed on patients who are older than 65. Although for every case physicians estimate operative risk, their predictive tools are limited and focus on a single organ system or solitary event. Another important fact to consider is that chronological age does not always match physiological age, and elderly people may vary widely from fit to frail at every age. "The ASA classification is highly subjective or quite arbitrary. Although it changed in 1962, 1980, it was originally introduced to clinical practice 70 years ago. At that time, geriatric population was a negligible number especially in surgical field but not now," Kim told Medical Daily.
Having decided to design a new model for assessing outcomes in older surgical patients, the team of researchers began by enrolling 275 patients over the age of 65 who were undergoing intermediate- or high-risk elective surgical procedures. Next, the team created a new model based on the comprehensive geriatric assessment (or CGA), which is widely used by doctors to detect disabilities and conditions associated with frailty in geriatric patients. Along with the CGA, the team of researchers analyzed specific patient characteristics as well as select laboratory variables.
Following surgery, many of the patients fared well, but others, not so much. Twenty-five patients (9.1 percent) died, while 29 patients (10.5 percent) experienced at least one post-surgical complication. Another 24 patients (8.7 percent) had to be discharged to nursing facilities.
Crunching the numbers on data collected both pre- and post-surgery, the team of researchers discovered certain distinct patterns. For example, malignant disease and low serum albumin levels were more common among the patients who died. Other factors, including dependence in activities of daily living, dementia, risk of delirium, short mid-arm circumference, and malnutrition were also identified as links to increased risk of death.
“A multidimensional frailty score model composed of the above items predicted all-cause mortality rates more accurately than the American Society of Anesthesiologists classification,” wrote the authors in their conclusion. Based on their results, the researchers believe their new model would be a more useful tool — compared to the current methods — to help physicians and surgeons predict those patients most likely to survive (and thrive!) following geriatric surgery.
Source: Kim S-W, Han H-S, Jung H-W, et al. Multidimensional Frailty Score for the Prediction of Postoperative Mortality Risk. JAMA Surgery. 2014.



























