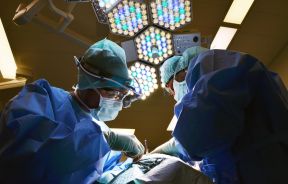
7000 Tulsa Dental Patients Urged To Seek HIV And Hepatitis C Tests

Tulsa, Oklahoma health officials urged 7,000 patients of a dentist based there to seek immediate medical attention to test for Hepatitis C and HIV after it was found that a local dentist's office was not properly sterilizing tools and equipment, even though he know several of his patients carried infectious diseases.
"It's uncertain how long those practices have been in place," said Kaitlin Snider, a spokeswoman for the Tulsa Health Department. "He's been practicing for 36 years.
The dentist under investigation, Dr. W. Scott Harrington closed his office and is cooperatin with health inspectors and authorities. He may lose his license to practice dentistry because of major violations of the Oklahoma Dental Act. He is set to appear for a hearing before the state Dental Board on April 19.
Letters were being sent to close to 7,000 patients who had been in the dentist's chair since 2007. The letter recommended patients go to their doctor for testing for HIV, Hepatitis B and Hepatitis C. Testing will also be offered free of charge at the Tulsa Health Department's North Regional Health and Wellness Center.
The case came to light when authorities were investigating a Hepatitis C case and found many safety violations. These included contamination of instruments used for different patients, even those known to have infectious diseases. A machine used to sterilize tools and equipment in the office was not functioning properly and may have allowed the spread of infectious material from patient to patient.
While HIV cannot survive for more than a few seconds outside of the body, according to the Center for Disease Control and prevention Hepatitis B can survive outside the body at least 7 days. During that time, the virus can still cause infection if it enters the body of a person who is not infected. Additionally Hepatitis C can survive on surfaces for at least 16 hours and as long as 4 days.
There are laws in place to prevent such risks from happening. All medical tools and devices are required to be sterilized after use and between patients in order to kill any pathogens.
According to the CDC "Based on limited studies, the estimated risk for infection after a needlestick or cut exposure to Hepatitis C-infected blood is approximately 1.8%. The average risk for HIV infection after a needlestick or cut exposure to HlV-infected blood is 0.3% (about 1 in 300). Stated another way, 99.7% of needlestick/cut exposures to HIV-contaminated blood do not lead to infection."
The best way to assure that your doctor or dentist is using proper procedure between patients is to ask if they properly sterilize tools between use. Dentists are supposed to undergo regular inspections by health officials to make sure that all protocols are followed and patients remain safe.
Published by Medicaldaily.com