Anal Cancers In U.S. Triple Since '70s
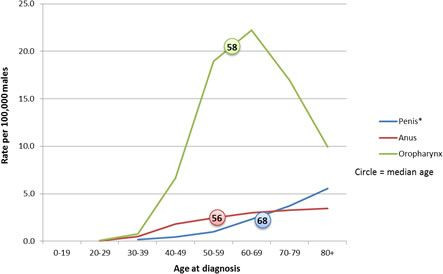
Anal cancers have tripled in the United States since the 1970s, particularly among men.
Researchers conducted a database search to find that the rate of anal cancers rose dramatically from approximately one in 100,000 people between 1973 to 1996 to three people per 100,000 from 1997 and 2009. The jump may be partially explained by better diagnoses.
"I think the literature has already shown that there has been an increase in anal cancer cases but we were surprised to see how dramatically it increased," said Dr. Lily Lai, of City of Hope in Duarte, CA, in a Reuters report.
Though both men and women experienced a rise in anal cancers, most of the increase was seen in men. Lai said the large increase in men might be due to more screenings, particularly among men with HIV. In the study, Lai and her colleagues analyzed in more than 11,000 squamous cell carcinoma cases found in a database of U.S. cancer cases through those years. Investigators found a particularly large increase in 1997, with more than 7,000 anal cancers diagnosed that year in comparison to some 4,200 nearly a quarter-century earlier.
By 1997, the rate of anal cancers in men had risen from one in 100,000 to three per 100,000, compared to a jump in women from 1.4 to 2.4 per 100,000. This year, the American Cancer Society projects that 7,000 people in the U.S. would be diagnosed with the cancer, resulting in 900 deaths.
The researchers reported in the Journal of Clinical Oncology that HIV-positive people tend to develop persistent human papillomavirus infections, which in turn are linked to the development of cervical and anal cancers. Eighty-percent of anal squamous cell carcinomas-the most common form of anal cancer-are caused by HPV.
"It could be that there is an increase in men (with anal cancer) and that there are other factors that we don't know are involved," Lai said. "We think it's probably a detection bias; that's the simplest explanation."
Dr. Robert Cima, a surgeon at the Mayo Clinic's department of colon and rectal surgery, said primary care physicians should identify patients with the highest risk levels for screening.
"...[C]ertainly a patient without risk factors is at very low risk for developing this kind of cancer, and a blanket screening program across the country for all patients would not be a useful approach," said Cima, who was not involved in the analysis.
Published by Medicaldaily.com



























