Cefaly, Device For Migraines, Receives FDA Approval Despite Lackluster Performance In Testing
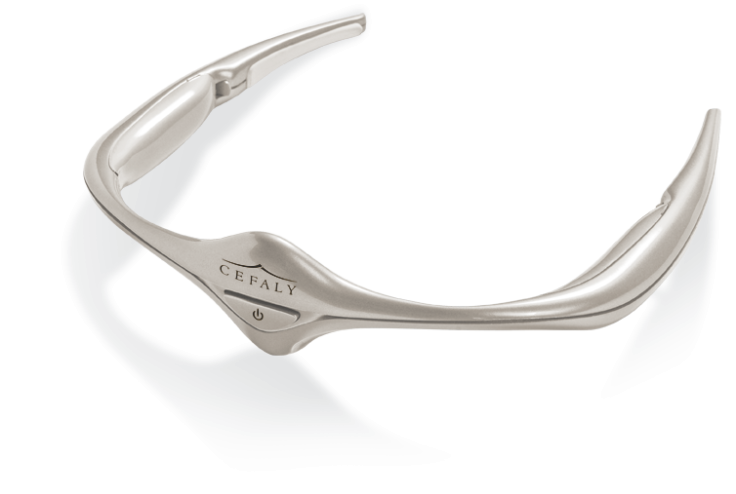
Cefaly, a new transcutaneous, tiara-shaped device used to treat migraine headaches received formal approval from the Food and Drug Administration (FDA) on Wednesday.
The agency green-lighting the device comes on the heels of a small, 67-person study conducted in 2012, in which 38 percent of subjects saw at least a 50 percent reduction in migraines in the experimental group. In the placebo group, roughly 12 percent of people saw a 50 percent reduction the number of migraines. Overall, the researchers found a “therapeutic gain” of 26 percent, which roughly means that for every three people that use the device, one person should expect migraine relief half the time.
“Cefaly provides an alternative to medication for migraine prevention,” said Christy Foreman, director of the Office of Device Evaluation at the FDA’s Center for Devices and Radiological Health, in an agency news release. “This may help patients who cannot tolerate current migraine medications for preventing migraines or treating attacks.”
Critically speaking, migraines are closer to seizures than to ordinary headaches. They’re classified as a chronic neurological disorder, finding roots in both the genetic and the environmental. Some 10 percent of the global population suffers from migraines, and they can last anywhere from two hours to three days.
Science hasn’t pinned down the exact mechanism that makes migraines so painful, but they speculate that an abnormally excited cerebral cortex mixed with ill-firing pain neurons makes for the splitting sensation. Cefaly is designed to stimulate the branches of the trigeminal nerve — suspect number one when it comes to migraines, sitting right behind the forehead. Users place the battery-operated headband on an adhesive electrode for 20 minutes, no more than once a day.
The 2012 study included migraine sufferers who experienced more than two attacks per month and who hadn’t used medication to treat the migraines for more than three months prior to using Cefaly. While overall migraine prevalence reduced marginally, when subjects did get migraines they were just as bad as without medication. And between the first use and the three-month mark, subjects saw a tiny (but statistically significant) drop in the number of migraine days, from 6.94 to 4.88.
What’s more, a separate study of patient satisfaction, including 2,313 Cefaly users, found 53 percent of people were happy with the product’s performance. The most common complaints involved the stimulation’s unpleasant feeling, sleepiness during the treatment, and headaches after treatment.
"New therapies are needed” in migraine research, wrote Dr. Eishi Asano, associate professor of pediatrics and neurology at Wayne State University, in a related editorial, “And further studies of neurostimulation using innovative study designs are warranted to explore the optimum way to create an acceptable evidence base for widespread use of this potentially valuable treatment.”
In other words, we can do better than 12 people having 50 percent fewer migraines, especially when 700,000,000 people’s mental health is at stake.
Published by Medicaldaily.com



























