Childbirth Position Sees Increased Blood Flow With More Pelvic Tilt: Have We Been Wrong All Along?

How could something as ancient and basic as childbirth go wrong? Surely we’ve figured that one out by now. Researchers aren’t so sure. A new study suggests the typical angle at which most obstetricians position their patients may be sub-optimal for promoting healthy blood flow during childbirth.
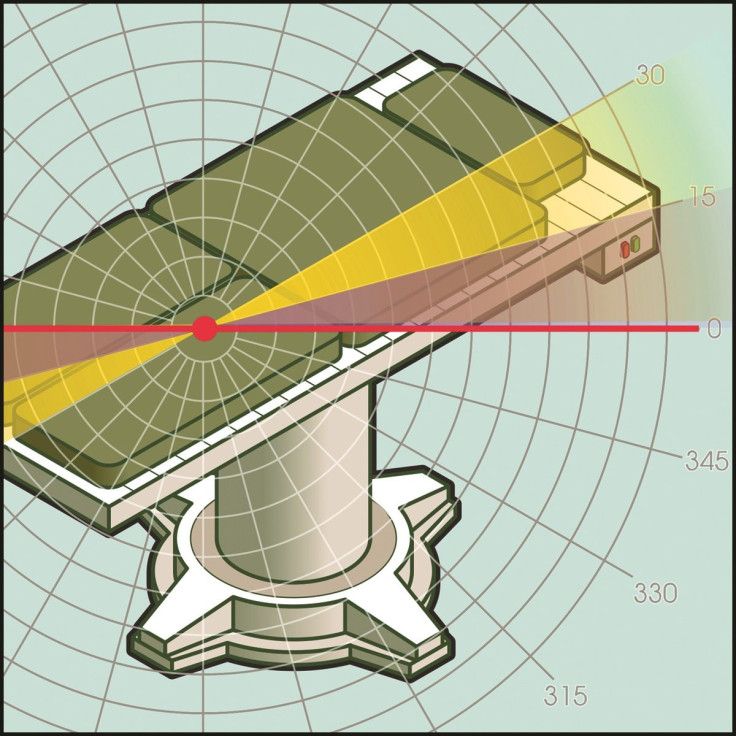
The new study, conducted by a group of physicians from Tokyo Women’s Medical University, in Japan, found the normal angle of tilt — 15 degrees — offered no discernable benefit to the women they studied. The only angle that seemed to take the pressure off the women’s inferior vena cava, a major vein located near the abdomen, was an angle of 30 degrees. The tilt relieved them of the pressure exerted by the fetus pushing on the vein.
“It is accepted by many physicians that positioning women on their side, with hips tilted at 15 degrees, during childbirth reduces this complication,” said Dr. Hideyuki Higuchi, study author from the University’s department of anesthesiology, in a statement. “However, our research found no evidence of aortic compression in pregnant women in any position and the recommended degree of tilt that most physicians follow did not reduce compression of the inferior vena cava at all. This is the first study to challenge this antiquated practice.”
Higuchi and his colleagues recruited 20 women, 10 at full term pregnancy and 10 who were not pregnant, to sit inside an MRI. Images from the scanner showed blood flow levels to the women’s inferior vena cava at each angle: flat on their backs and at 15, 30, and 45 degrees. Regardless of the position they were put in, both groups saw no decrease in blood flow in the desire vein or decrease in size in the abdomnial aorta — the only difference being a near total loss of circulation when pregnant women lay flat on their backs.
Childbirth doesn’t come with just one accepted theory, but multiple theories. Some women choose to experience a water birth, delivering their child fully submerged to ease the transition from the womb. Others change their positioning to make themselves more comfortable and let them push more easily. These include resting on all four limbs, squatting, lying on their side, or standing at certain angles. The new evidence seems to say all those methods could be valid, but the most conventional method — sitting relatively upright — needs some rethinking.
In a related editorial, Dr. Craig Palmer, professor of anesthesiology at the University of Arizona, agreed the findings are certainly set to be disruptive. On the upside, they should get the medical community questioning whether the accepted practices are the best ones. However, the road to full implementation may be tricky, especially in special-needs cases.
“Although it would be great to be able to conclude by saying all of our patients in the delivery room should be placed in at least 30 degrees left lateral tilt after regional anesthetic,” Palmer said, “I have serious doubts that our obstetric colleagues would find it a reasonable position for cesarean delivery, particularly in obese patients.”
Nevertheless, he expressed overall acceptance of the new information. Anything that gets patients delivering their children in a safer environment is probably a practice that deserves widespread attention, he said. “Kudos to the authors of this study for revisiting an 'ancient' practice, applying current technology to the matter, and shedding new light on an old routine.”
Correction: A previous version of this article incorrectly referred to the inferior vena cava as an artery, not a vein.
Published by Medicaldaily.com



























