Finding a New Virus: Spit, Sequencing and Serendipity
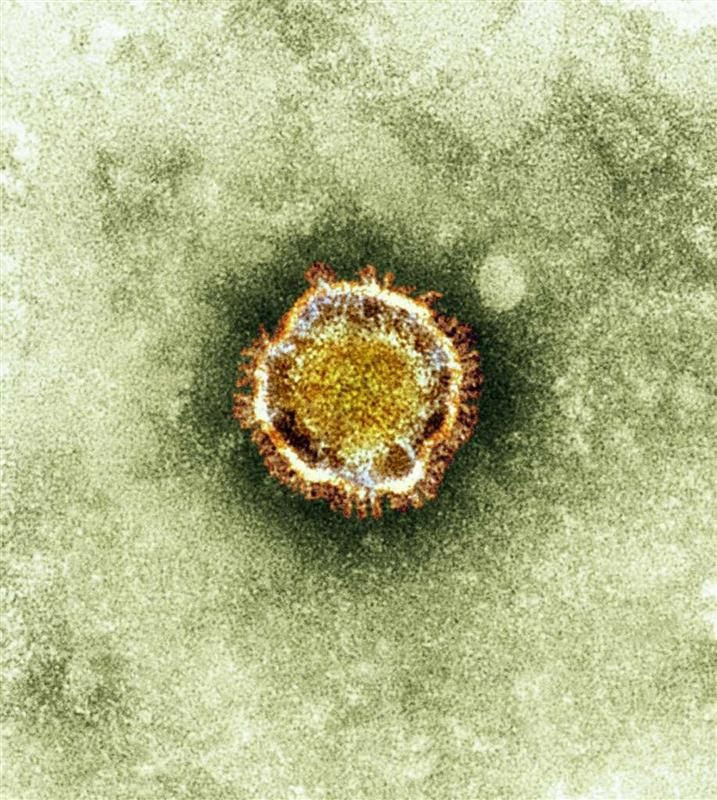
Professor Maria Zambon's first thought when her team of scientists matched a virus from a patient's sputum to one never before seen in humans was: "Oh no, this is going to be tricky."
In her north London laboratory last Saturday, an email came in from another specialist virology team in The Netherlands with a 99.5 percent match to a virus from the same family as SARS, a disease that emerged in 2002 and killed 800 people. Her thoughts moved swiftly to the risk of an international outbreak.
"Of course it's really interesting scientifically to get this kind of result, but you also think about what it might mean," she said in an interview. "Is this the tip of an iceberg? Or is this an isolated event?"
At this stage neither Zambon, who is director of reference microbiology at the UK Health Protection Agency (HPA), nor her team, nor their collaborators at the Rotterdam Erasmus Medical Centre, nor any World Health Organisation (WHO) expert, knows the answer.
But they're working on it.
Speeding them along in that effort are state-of-the-art technologies that allow scientists to decipher the genetic makeup of a virus in a matter of hours - work that a decade ago would have been only just possible, and far slower.
Five days after finding that the patient, a Qatari man in intensive care at a London hospital, had a previously unknown virus from a family called coronaviruses, Zambon's team had sequenced part of its genome, mapped out a so-called "phylogenetic tree" of its links, and published it all online.
"We've done something pretty unique here in terms of early disclosure of data and making the sequence available to the global community incredibly quickly," said Zambon. "That will help people working in diagnostic laboratories worldwide."
With any emerging disease, as with H1N1 swine flu and bubbling concerns about bird flu mutating and spreading between humans, the fear is that scientists will be chasing a disease, unable to develop drugs or vaccines fast enough to contain it.
SARS, or Severe Acute Respiratory Syndrome, was also new when it emerged in China in 2002 and went on to kill around a tenth of the 8,000 people it infected. But experts stress it was transmissible among people - something that seems so far not to be the case with this virus.
The WHO stresses there are only two confirmed cases of the new virus worldwide and several laboratories, including Zambon's, are already developing rapid tests.
SPIT AND SERENDIPITY
The story of how Zambon's team got to this stage is one of smart scientific detective work, timely checking of emails and a bit of serendipity. But it starts right back at the basics, with a call from a worried doctor and some spit.
"Fresh secretions - basically sputum, or spit - were obtained" from the patient, Zambon explains, after an initial call from doctors treating the Qatari man caused scientists in her lab to be concerned he might have a rare infection.
"If you're a virologist in a laboratory like ours and handing clinical material, whether it be human on animal, you always have to be alive to the possibility that once in a while you might turn up something unusual," she said.
Maybe because of that, it happened that two key HPA scientists had both spotted a post on an internet-based reporting system called ProMED-mail - the Program for Monitoring Emerging Diseases.
That post, headlined "Novel Coronavirus - Saudi Arabia" came from Dr Ali Mohamed Zaki in a lab at Soliman Fakeeh Hospital in Jeddah and described a 60-year-old man who died in July of severe respiratory infection and kidney failure.
Zaki sent samples from this patient to Professors Ron Fouchier and Ab Osterhaus at Erasmus - a highly respected virology team made world famous earlier this year for its work on mutations of bird flu viruses.
Having been alerted to the proMED post, Zambon emailed Osterhaus and Fouchier in the Netherlands.
"Clearly Ab checks his email on Saturdays, because he called me 20 minutes later and I told him the situation," said Zambon.
A battery of tests on the Qatari patient's sample had come up with an unusual pattern - negative for all known human coronaviruses, including SARS, but positive on a catch-all test. This was a strong indication the virus was from that family.
"That's when you realise you've got funny result and you need to do something more," said Zambon.
The team set about sequencing a "tiny snippet" of the virus' genome, then moved on to a so-called a "blast analysis" to see if they could find a match.
"You literally blast the sequence fragment you've got against everything else that's publicly available," Zambon explained. "That provides an alignment of your sequence with other known sequences to give you a measure of identity."
At this point, "the information came back that it was 99.5 percent identical with the Dutch team's virus" Zambon said.
The chain of events from that point, late in the London day on Saturday 22, saw the HPA immediately reporting their find to the WHO, which in turn issued a global alert about the new virus late on Sunday evening.
Within hours, Zambon said, the HPA was facing "a rising tide of requests" for information about how to spot, test for and diagnose the virus - which it hopes to answer as best it can the DNA analysis data and phylogenetic tree information online.
As she and other scientists work on finding out more, Zambon praises the sharp minds and eyes of her team.
"But I admit I'm tempted to say to them the next time they have a smart idea on a Friday afternoon: 'Just hold it until Monday morning'."
Published by Medicaldaily.com



























