In-Hospital Cardiac Arrest Care Varies Among US Hospitals; Following Guidelines Could Save Lives
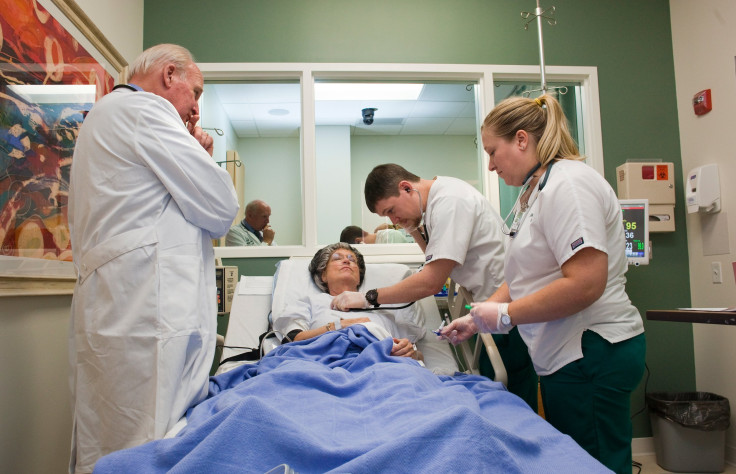
In-hospital cardiac arrests (IHCA) are responsible for over 200,000 incidents annually in the United States. Though the American Heart Association has put out a set of recommended care measures, many U.S. hospitals are not following them, according to a new study published in JAMA Cardiology.
Hospitals across the U.S. vary in terms of the rates at which patients who have cardiac arrests while admitted survive long enough to be discharged. It’s unknown whether these varying rates are due to differences in care quality, but some specific measures, such as taking less time to provide defibrillation, are associated with better patient survival. The findings included in the current study showed that patients treated at hospitals with greater adherence to the recommended guidelines have a better chance of leaving the hospital.
Dr. Monique L. Anderson, of Duke University Medical center, used data from the American Heart Association’s Get With the Guidelines-Resuscitation (GWTG-R) program, allowing her and her colleagues to analyze 35,283 patients with IHCA treated at over 250 hospitals across the country from 2010-2012. The researchers calculated a performance score for IHCA for each patient, based on five measures the guidelines recommend.
After adjusting for variables, the team found each 10-percent increase in a hospital’s performance in treating the cardiac arrest was associated with a 22 percent higher chance of survival for the patient. A higher hospital performance score was also associated with a favorable neurologic status for the patient at discharge.
If all hospitals operated at the level of the highest-performing hospital, researchers said, an estimated additional 22,990 to 24,200 lives could be saved every year.
“Although this is an estimate only, it helps to shed light on the effect of ensuring timely and high quality care for IHCA,” the study reads. “Significant opportunities remain for improving adherence to guideline-recommended care overall and with individual process-of-care measures. Of importance, enhancing process quality of care may improve outcomes for the many patients with IHCA.”
IHCA is not the first area in which hospitals have slacked on implementing the recommended guidelines. A December 2015 study found many hospitals’ policies for determining brain death are inconsistent, and some hospitals have failed to implement guidelines created to reduce errors and harm done. There has also been trouble in the cancer world — guidelines for PET use in recovering lung cancer patients have been flouted in many institutions, and the colon cancer screening guidelines have been questioned for allowing too many cases to go unnoticed as well.
Source: Anderson M, Nichol G, Dai D, Chan P, Thomas L, Al-Khatib S, et al. Association between hospital process composite performance and patient outcomes after in-hospital cardiac arrest care. JAMA Cardiology. 2016.
Published by Medicaldaily.com



























