Psoriasis Patients Are Unhappy With Current Treatments; Are Health Insurance Constraints To Blame?
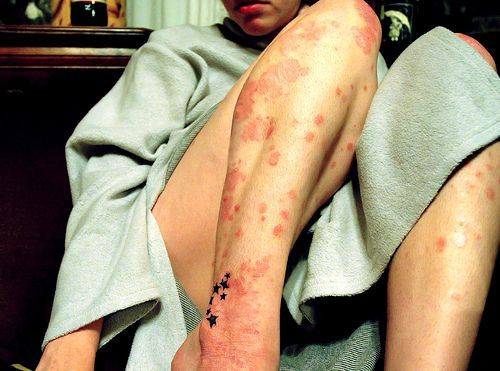
Over half of psoriasis patients said they are unhappy with the treatment they’re receiving for the immune-mediated skin condition, finds a new study published in JAMA Dermatology.
Researchers at University of California, Davis compiled data from 2003 to 2011 on people with psoriasis and psoriatic arthritis — a rarer condition resulting from joint inflammation — finding that out of 5,604 total cases, 30 percent of people with severe psoriasis were receiving no treatment at all, with proportions rising in mild and moderate cases. Lead researcher Dr. April Armstrong said these figures point toward ineffectiveness and inaccessibility in many of the latest treatment options.
"Much More Than A Cosmetic Condition"
“The high proportion of patients who are not being treated, or are being inadequately treated, is a concern because psoriasis is much more than a cosmetic skin condition.” said Armstrong, associate professor of dermatology at UC Davis. “It’s a serious and chronic medical disease.”
Psoriasis has somewhat of a controversial title, as some experts assert that its status as an autoimmune disease actually muddles the term’s definition, as autoimmune diseases typically involve the host’s body confusing outside antigens as normal body components, and attacking them both. Psoriasis seems to differ in the way it is caused — not by outside antigens, but by clusters of immune cells that send signals to one another and coordinate inflammation that way. Diagnosis takes place upon skin observation; no blood tests need to take place, though biopsies are routinely taken.
In treating the condition, doctors have several paths they can follow. Mild to moderate cases of psoriasis typically see the greatest benefit from topical agents, such as bath solutions, moisturizers, mineral oil, and petroleum jelly to keep the skin from drying out. Medicated ointments may be used to reduce inflammation, remove dead skin, and clear affected skin of plaques.
“Psoriasis afflicts about 7.5 million Americans and is responsible for over 11,000 cardiovascular disease deaths each year in the U.S.,” said Armstrong, highlighting psoriasis patients’ increased risk for heart attack, diabetes, and premature death.
Stronger cases of psoriasis find treatment in medication specially designed to interrupt the coordination put on by immune cells. These medications are called biologics, and popular brand names include Enbrel (etanercept) and Humira (adalimumab). Most people involved with Armstrong’s study, however, stopped use of the medication because they said it didn’t work. Thirty percent of patients with moderate psoriasis and 22 percent with severe cases said they were on topical treatments alone.
Overcoming Financial Obstacles
The problem is, obtaining the more powerful medication requires some maneuvering on the part of health insurance companies. For the patient, covering the yearly cost of such drugs can be an insurmountable obstacle, as treatments run for as much as $25,000 a year. Andrew Robertson, chief medical and scientific officer for the National Psoriasis Foundation, said it’s for this reason under-treatment rates could be so high, a view with which Armstrong agrees.
“We want payers to understand the serious medical consequences of non-treatment and under-treatment of psoriasis and psoriatic arthritis,” Armstrong said. “There are also psychiatric consequences to these conditions. Patients often become depressed and some even suicidal because their quality of life is so poor.”
A 50 percent dissatisfaction rate for psoriasis patients and 40 percent dissatisfaction rate for psoriatic arthritis patients come in part from lack of patient awareness about the condition’s chronic nature, Armstrong added. Patients who stay on medication with minimal improvements grow frustrated that these benefits don’t last. Even during clinical treatment, symptoms can come and go, she said.
Mark G. Lebwohl, the study’s senior author and professor and chair of dermatology at Mount Sinai Medical Center in New York City, conferred the supposed benefits of biologics with Armstrong. Phototherapy has also been shown effective in treating psoriasis; however, high co-payments and low reimbursement rates from insurance companies prevent many doctors from performing the procedure.
“Unfortunately, there are real barriers that prevent patients from being treated,” said Lebwohl. “Nearly every practicing dermatologist in the U.S. has written a prescription that has been denied by an insurance company.”
Source: Armstrong A, Robertson A, Wu J, Schupp C, Lebwohl M. Undertreatment, Treatment Trends, and Treatment Dissatisfaction Among Patients With Psoriasis and Psoriatic Arthritis in the United States. JAMA Dermatology. 2013.
Published by Medicaldaily.com



























