Should Breast Cancer Patients Skip the Pre-op MRI?
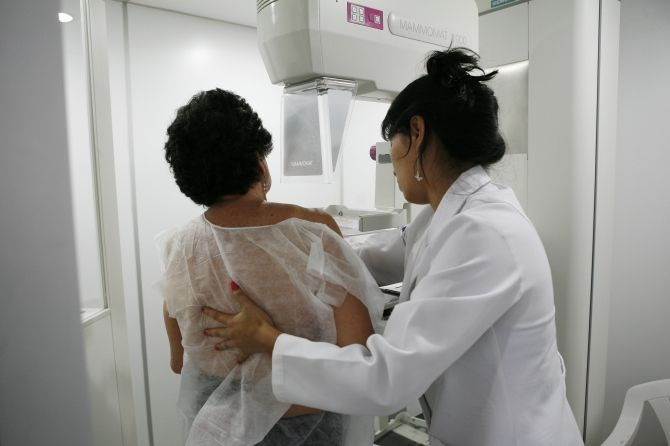
A new review of existing evidence suggests that using magnetic resonance imaging to "stage" a woman's breast cancer before surgery might do more harm than good.
MRI produces a much clearer image than X-rays and ultrasound, and is recommended for detecting early tumors in women at increased risk for breast cancer. But routinely using the technology once any woman is diagnosed with a tumor may lead to more radical surgery without any benefits, says a team of Australian and U.S. researchers.
They found that about 26 percent of women who had a pre-operative MRI to help determine the extent and severity of their tumor ended up having their entire breast removed, compared to about 18 percent of those whose surgeons only used traditional methods of characterizing the cancer.
"I wasn't surprised by the results at all. What I am surprised by was the strength of the data," said Dr. Monica Morrow, the study's senior author and the chief of breast service at Memorial Sloan-Kettering Cancer Center in New York.
Because MRIs are more sensitive than mammograms, some doctors think they are a good tool for identifying the precise outlines of cancerous tissue. Others, however, have begun to question whether the imaging led surgeons to remove more breast tissue than necessary.
Moreover, women who have MRIs before breast surgery seem to be no less likely to need a second surgery to remove additional cancerous tissue.
A study published in September, for instance, found that among more than 300 women who underwent breast cancer surgery, just as many of those who had an MRI before the first surgery ended up having a repeat operation.
An MRI can also add more than $1,000 to a patient's bill.
"I think more surgeons are starting to question this because they're seeing the outcomes," Morrow said.
For the new study, she and her colleagues pulled together data from nine previous studies to see if MRIs influenced the number of women who had their breast removed or who had a second surgery to remove additional cancer.
From the nine studies, the researchers had information on 3,112 women who had breast cancer surgery.
Overall, the team found that about 16 percent of the women who had an MRI ended up having the entire cancerous breast removed, known as a mastectomy, during their first surgery. That's compared to about 8 percent of women who did not have an MRI.
They also found that having an MRI before surgery did not influence whether women would need additional surgery to remove more tissue. In each group, between 11 percent and 12 percent had to go back under the knife.
After taking into account the women's initial surgery and the second operations, the researchers calculated that about 26 percent of those who had an MRI ended up having their entire breast removed, compared to 18 percent in the no-MRI group.
"It causes more mastectomies to start with, but it doesn't decrease the number of women who started out wanting a lumpectomy and needing a mastectomy," said Morrow of preoperative MRIs.
The study did not look at long term outcomes, including how many women survived beyond five years. Nor did it examine the use of MRI to screen the opposite breast for signs that cancer had spread, the researchers note in their report, which is published in the Annals of Surgery.
These results do not apply to certain subgroups of patients, they add, including women with genetic mutations that predispose them to cancer and those whose other diagnostic tests produced conflicting results.
But based on the short term measures of how many surgeries women got and how much tissue surgeons removed from them, Morrow told Reuters Health that MRIs do not seem to have a place in breast cancer surgery.
"There may be select circumstances where we'd use it to solve a problem, but for most women with breast cancer they don't need an MRI for their evaluation," she said.



























