Sleep Helps Babies Learn, Adults Declutter the Brain
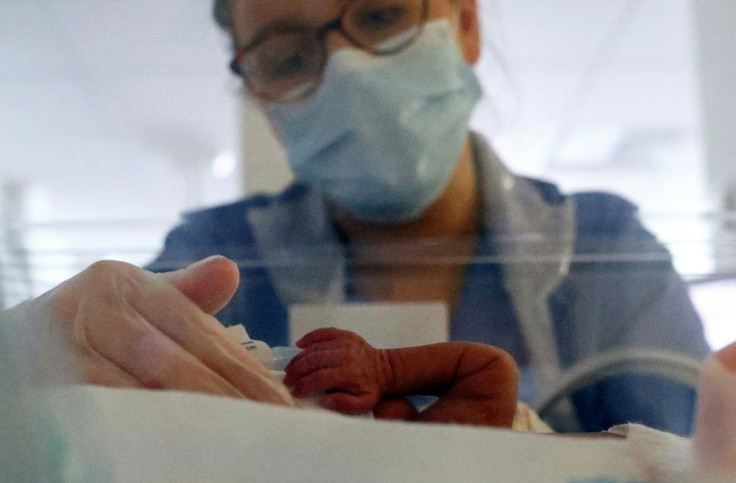
A new study led by Van Savage, PhD, a professor at the University of California, Los Angeles (UCLA) suggests that deep sleep, known as REM (rapid eye movement) sleep, is used differently by a baby’s growing brain and an adult’s mature one.
The researchers, who looked at data from dozens of sleep studies involving humans and other mammals, confirmed that babies up to the age of 2½ need REM sleep for their brains to develop. Around 2½ years of age, this activity abruptly stops. From that age until we die, the brain uses the period of REM sleep to repair the brain, trimming nerve connections and cleaning up the debris.
Babies are in REM for 50% of their sleeptime. The brain spends most of that time growing and making new connections. By 10 years of age, the amount of sleep spent in REM decreases to around 25%; it further decreases to 15% for adults over the age of 50.
Do brain development and clean-up suffer during sleep deprivation or decreased time in REM sleep?
Jeffery Kingsley, MD, a pediatrician at Valley Children’s Hospital in Madera, Calif., suggests that if an infant were to miss some REM sleep, “REM will take what it needs from other parts of the sleep cycle.” Even if the infant loses out on REM due to illness, by 2 ½ years of age all babies are at about the same stage of development. The exception is children who have been diagnosed with developmental issues or disability.
Dr. Kingsley works with premature infants and described how an infant who is born at 34 weeks can look pretty much like a full-term infant born at 40 weeks. But the premature infant will be too tired to eat about 24 hours after birth and will need to be fed through a feeding tube. Then, after several days, like “flipping a switch,” the baby will be irritated by the tube in the back of the throat and start crying.
“We take the feeding tube out and the baby can suddenly suck and swallow,” Dr. Kingsley told Medical Daily. He believes that this supports the researchers’ claim that babies’ brains are continuing to grow even after they are born.
Although there are only two types of sleep – REM and NREM (non-REM) – there are four stages in the sleep cycle: three NREM stages and one stage of REM.
During the three NREM stages, the body is moving from wakefulness to deep sleep. REM is deep sleep; the eyes move from side to side. Dr. Kingsley describes REM as “like being in a movie.” The brain is reviewing things that happened while awake and is reorganizing connections. Both REM and non-REM are important for learning and memories.
The researchers believe that being awake damages parts of our brain, and this damage must be reversed, repaired and cleaned up while we are in REM sleep.
Microglia is the name of the brain’s “Pac-Men,” who patrol the brain looking for and gobbling up infections and dead cells that have been trimmed from brain connections during the repairs.
Some researchers suggest that as we age our sleep is broken up, which might decrease the ability of the microglia to clean up. This leaves behind debris that might contribute to the cognitive decline experienced by older adults.
Wendy Zachary, MD, is a geriatrician and medical director of the Acute Care for the Elderly (ACE) Unit at California Pacific Medical Center (CPMC) in San Francisco. The ACE Unit is where patients who are 70 and older are cared for when admitted to CPMC. This unit plans and provides specialized care for elderly patients who have geriatric syndrome.
It is well known that long-term sleep disturbance can lead to delirium and cognitive impairment. Many of the elderly patients that she sees have been on medications to help them sleep for decades. Many people also self-medicate daily with alcohol or over-the-counter medications. Unfortunately, sleep medication prescribed years ago may now be too strong for the elderly person.
“Aging is hard. There are so many changes to our body,” Dr. Zachary told Medical Daily. The kidneys don’t work as well as they used to. They get rid of less of the medication, so it is still in the system when the person wakes up the next day. She might feel groggy and fall and break a hip or end up with a head injury. Grogginess might also lead to napping that interferes with nighttime sleep.
One goal of the ACE unit is to decrease or eliminate the dependency on drugs for sleep. Activities that engage the patient during the day help to stave off boredom. Mobility is encouraged so that the person has less inclination to take a nap. These activities help the patient to feel sleepy at bedtime and can lead to longer periods of sleep at night, so the sleep/wake cycle can be restored.
With better sleep at night, the repairs, decluttering and brain “garbage” removal can take place for longer periods. The less groggy, more active patient can return home in better shape than when she arrived.
Because REM sleep is so important for all age groups, it is best not to wake up someone who might be in REM sleep. Regardless of age, the brain needs all the REM sleep it can get.
Yvonne Stolworthy MSN, RN graduated from nursing school in 1984 and has had a varied career. Many years were spent in critical care. She has been an educator in a variety of settings, including clinical trials. Currently she is applying her nursing knowledge to health care journalism.
Published by Medicaldaily.com