Surgeons Use CT Imaging And 3D Printing To Successfully Separate Conjoined Twins
3D printing has been instrumental to a variety of recent medical procedures, from giving a 3-year-old girl a new skull to creating a new rib cage for a cancer patient. It’s also allowed doctors to prepare for the delivery of a baby who would have otherwise experienced complications during birth. Now, in a study presented at the annual meeting of the Radiological Society of North America (RSNA), researchers have used 3D printing to help plan for the surgical separation of conjoined twins.
Conjoined twins develop in the womb during the early stages of pregnancy, when the embryo would normally separate into two. Instead, they remain attached, normally somewhere between the buttocks and the chest, sharing organs and blood vessels. One in every 200,000 live births in the U.S. is to conjoined twins, and separation is extremely difficult even as success rates have increased steadily — since 1950, at least one twin has survived a separation procedure about 75 percent of the time, according to the University of Maryland Medical Center.
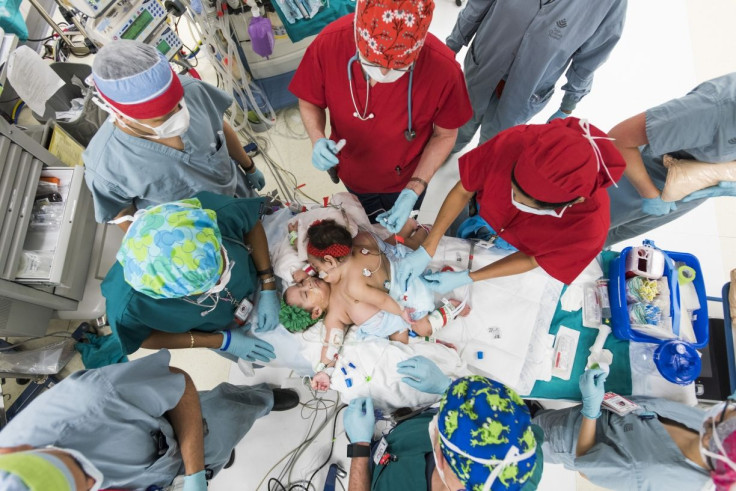
The subjects of the current study were Knatalye Hope and Adeline Faith Mata, conjoined twins from Texas who were born connected from the chest down to the pelvis on April 11, 2014. “This case was unique in the extent of fusion,” said lead author Dr. Rajesh Krishnamurthy, chief of radiology research and cardiac imaging at Texas Children's Hospital, in a press release. “It was one of the most complex separations ever for conjoined twins.”
To prepare for the risky operation, the surgeons used volumetric CT imaging with a 320-detector scanner, which essentially gave the surgeons more accurate and in-depth images of the twins’ bodies than they’d normally get with traditional CT scans. They gave each twin an intravenous contrast, a liquid that illuminates blood vessels, the skeletal system, and organs, so surgeons could get a clearer picture of the twins’ insides and determine which organs or blood vessels they shared. And finally, they used a technique called target mode prospective EKG gating to freeze the hearts’ movements in order to get a better look at the cardiovascular anatomy and reduce the twins’ exposure to radiation.
"The CT scans showed that the babies' hearts were in the same cavity but were not fused," Krishnamurthy said. "Also, we detected a plane of separation of the liver that the surgeons would be able to use."
The surgeons then used the images to create 3D-printed models of the twins’ skeletal structures and organs, designed to be assembled together or used separately — they also featured different colors to tell each twin apart. Not only was this useful for educating the doctors about the twins’ anatomy before the procedure, but it also helped them to communicate the procedure to the twins’ parents.
The operation took place on Feb. 17, 2015. Thanks to the 3D-printed models, the surgeons found "the landmarks for the liver, hearts, and pelvic organs just as we had described," Krishnamurthy said. Twenty-six hours later, the operation was done, and in May 2015 Knatalye went home. Adeline was sent home a month later.
Source: Krishnamurthy R, et al. Radiological Society of North America presentation. 2015.
Published by Medicaldaily.com



























