Teen Birth Control Use Is High, But Most Effective Forms Are Being Ignored
Teen pregnancy rates have been on the decline for a few years now, thanks in part to increasing awareness of the risks associated with unprotected sex. They’re still having sex, though, according to a new report from the Centers for Disease Control and Prevention (CDC), which found that 43 percent of those aged 15 to 19 have had sex. But while it’s a good thing the majority of them (86 percent) are using some form of birth control, the CDC found that very few of them are using the most effective forms.
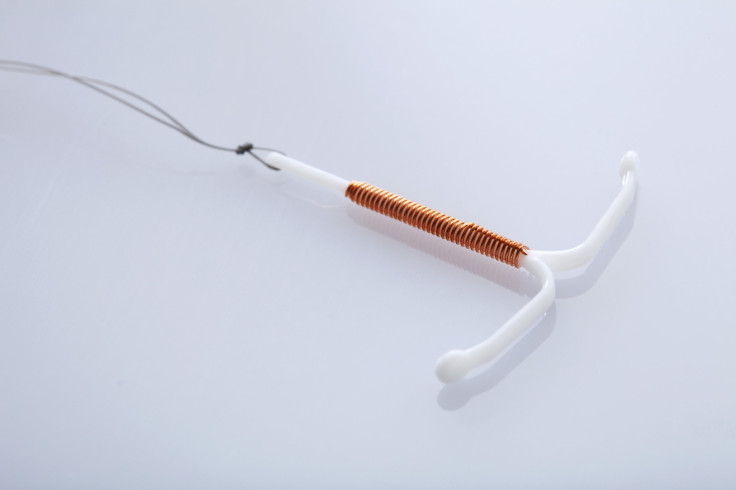
Those types of birth control, called long-acting reversible contraception, are intrauterine devices (IUDs) and implants. Both are inserted by a doctor into the arm or uterus, respectively, and stay there for three to 10 years. The CDC found that less than five percent of teens used these forms of birth control in 2013. And while the thought of a foreign object remaining in the body for so long might dissuade many women, IUDs and implants are not only the most effective form of birth control but also the safest. They require little maintenance, too.
IUDs and implants both have failure rates of less than one percent, meaning less than one in 100 women will get pregnant within their first year of using the devices. Both release the hormone progestin, which prevents eggs from leaving the ovaries and makes cervical mucus thicker, blocking sperm from moving through. Some IUDs also come with copper-wire wrapping that kills sperm cells. And because they work continuously for so long, women using them can focus their minds on other things.
By comparison, birth control pills and condoms, which teens use most often, have respective failure rates of nine and 18 percent. It’s simple why these rates are higher. Birth control pills require constant awareness; they should be taken every day at the same time. New condoms should be worn with each sexual encounter. Not only can both be used improperly, but it’s easy to forget to use them at all, especially when getting lost in the heat of the moment.
Educating teens about their options is the first step to increasing IUD and implant use, the researchers said. Many people believe the devices are still dangerous after 1970s versions of them caused pelvic infections. However, their quality has vastly improved, and recently, the American College of Obstetricians and Gynecologists and the American Academy of Pediatrics endorsed both IUDs and implants as a “first-line contraceptive choice for teens that can be combined with condoms to provide the best protection against pregnancy and sexually transmitted diseases.”
Beyond that, increased access and availability, as well as educating health care providers, will likely convince teens to be more proactive with their contraceptive methods.
Source: Romero L, Pazol K, Warner L, et al. Vital Signs: Trends in Use of Long-Acting Reversible Contraception Among Teens Aged 15–19 Years Seeking Contraceptive Services — United States, 2005–2013. Morbidity and Mortality Weekly Report. 2015.
Published by Medicaldaily.com



























