Bioengineered Blood Vessel Implanted In Virginia Kidney Dialysis Patient, An American First
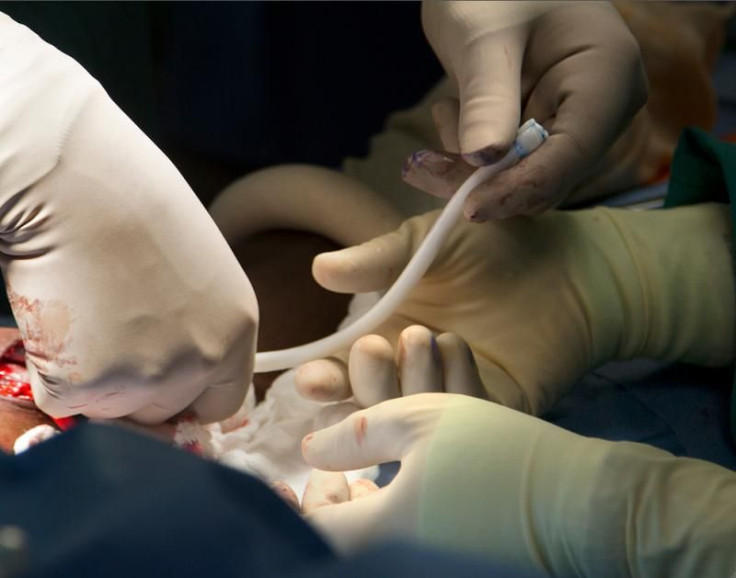
A bioengineered blood vessel implant in his arm has potentially given a 62-year-old Virginia man a new lease on life, after years of dialysis for end-stage kidney failure.
"This is a pioneering event in medicine," said Dr. Jeffrey H. Lawson, the Duke University School of Medicine vascular surgeon who helped develop the groundbreaking technology and carried out the surgery, in a news release. "It's exciting to see something you've worked on for so long become a reality."
The bioengineered blood vessel graft took place on June 5, a two-hour surgery that marked the beginning of the first American clinical trial to test the safety of lab-grown vein implants.
Building a Bioengineered Blood Vessel
Researchers at Duke and an affiliated bioengineering company called Humactye built the blood vessel by growing human smooth muscle cells on a tube-shaped biodegradable mesh scaffold. The structure was immersed in a bath of vital amino acids, with pulses of energy pumping nutrients in a heartbeat rhythm mimicking the physical forces that shape natural blood vessel growth.
The resulting collagen vein structure was then rinsed in a solution to wipe away biological cell properties that could trigger an immune response, leading to organ rejection.
Making the blood vessel nonreactive can allow it to be mass-produced in a matter of months, said the researchers, saving the time and energy that it would take to harvest an individual patient's own cells to seed a personalized vein structure.
"At the end of the process, we have a non-living, immunologically silent graft that can be stored on the shelf and used in patients whenever they need it," said Dr. Laura Niklason, the co-founder of Humacyte, in the news release.
The blood vessel implants are flexible and life-like, said Dr. Niklason, unlike stiffer artificial vein replacements made of materials like Teflon or Dacron. They are designed to take on the cellular properties of their host's native tissues, and eventually become impossible to tell apart from living blood vessels.
"They are functionally alive," said Dr. Lawson. "We won't know until we test it if it works this way in humans, but we know from the animal models that the blood travels through the blood vessels and they have the natural properties that keep the blood cells healthy."
Such bioengineered veins were first implanted in clinical trials in Poland, which began in December 2012, after years of testing in dogs and baboons.
The Virginia patient marks the first American participant in a phase one clinical trial approved by the Food and Drug Administration (FDA), which will ultimately include 20 kidney dialysis patients.
Bionic Blood Vessels for Kidney Dialysis and Heart Bypass Surgeries
The purpose of the bioengineered blood vessel is to speed blood flow during hemodialysis, a procedure that externally filters wastes from blood after kidney failure.
Dialysis often requires a graft in the arm, but current implant options come with problems like frequent clotting for artificial blood vessel grafts, and heightened infection risk for veins harvested from different parts of a patient's own body, both of which raise the specter of repeat hospitalizations.
The Duke researchers' nonreactive bioengineered blood vessels could represent a significantly more stable alternative to the more than 320,000 Americans who require dialysis for kidney failure, or end-stage renal disease.
Such bioengineered blood vessels could also be developed into implants for heart bypass surgeries, which over 415,000 Americans undergo each year, and replacements for other blocked veins and arteries.
"We hope this sets the groundwork for how these things can be grown, how they can incorporate into the host, and how they can avoid being rejected immunologically," said Dr. Lawson. "A blood vessel is really an organ — it's complex tissue. We start with this, and one day we may be able to engineer a liver or a kidney or an eye."
Sources:
Dahl SL, Kypson AP, Lawson JH, et al. Readily available tissue-engineered vascular grafts. Science Translational Medicine. 2011.
Pritchard HL, Manson RJ, DiBernardo L, et al. An early study on the mechanisms that allow tissue-engineered vascular grafts to resist intimal hyperplasia. Journal of Cardiovascular Translational Research. 2011.
Sarnak MJ, Levey AS, Schoolwerth AC, et al. Kidney Disease as a Risk Factor for Development of Cardiovascular Disease. Hypertension. 2003.
Recovering from coronary bypass surgery. Harvard Heart Letter. 2012.



























