A Brief History Of Vaccines: From Medieval Chinese ‘Variolation’ To Modern Vaccination

Vaccines are an integral aspect of medicine; in the developed world, most children must undergo mandatory vaccinations in order to attend school. The average child is protected from diphtheria, hepatitis A and B, influenza, measles, mumps, polio and whooping cough — all diseases that were historically so hazardous they could easily wipe out thousands of people.
Most vaccines are created from either weakened or dead forms of the biological agents of the diseases themselves. Injecting small amounts of dead microbes into a person stimulates the immune system enough to create antibodies against them and destroy them; this serves as protection from the same microbes later on. Vaccines allow the immune system to maintain a record of the disease, which makes it easier to destroy those threats afterwards.
Vaccines are one of modern medicine’s miraculous breakthroughs — but they existed hundreds of years earlier in primitive forms, referred to today using the term “variolation.” Below is a brief history of vaccines, from the ruminations of ancient physicians to the modern war against Anti-Vaxxers.
Ancient
429 BCE. Though there was no knowledge of antibodies in ancient Greece, physicians at the time were beginning to understand that getting infected with certain viruses could later prevent re-infections. For example, in 429 BCE, Greek historian Thucydides recorded that people who survived the smallpox epidemic in Athens were safe from re-infection.
Medieval
900-1000 AD. The first precursor to a modern vaccination, however, occurred in China. The Chinese were the first to develop a primitive form of a vaccine around the 10th century, according to the NHS. Known as variolation or inoculation, the method was developed to prevent smallpox — a destructive disease that frequently plagued Europe and Asia in the Middle Ages. Chinese physicians discovered that when healthy people were exposed to smallpox scab tissue, they were less likely to get infected with the disease later on (or if they did, it was a much milder, less dangerous version). The most common form of inoculation in China was to crush smallpox scabs into powder, then breathe it in through the nose.
Modern

Early 1700s. Until the 18th century, inoculation was a practice largely confined to China, India, Turkey, and other eastern countries. Lady Mary Montagu, an aristocrat and the wife of England’s ambassador to Turkey, is credited as being the first to bring attention to the practice in the Western world. In 1715, Montagu had gone through her own bout of smallpox, and had been disfigured as a result. After learning about inoculation during her time in Turkey, she was determined to protect her six-year-old son from the disease through inoculation.
“The smallpox, so fatal, and so general amongst us, is [in Turkey] entirely harmless by the invention of [inoculation],” Montagu wrote to a friend. “There is a set of old women who make it their business to perform the operation every autumn… The old woman comes with a nut-shell full of the matter of the best sort of smallpox, and asks what veins you please to have opened…”
In 1721, Montagu had her two-year-old daughter inoculated, marking the first inoculation in England. News of the practice began to spread and be accepted by Western European physicians, though many people remained skeptical. Smallpox inoculation was still dangerous and killed about 2-3 percent of those injected with small amounts of the virus.
1742. In Letters on the English, Voltaire wrote about inoculation in the hopes of convincing his fellow French people to embrace the method. “The Circassian women have, from time immemorial, communicated the small-pox to their children when not above six months old by making an incision in the arm, and by putting into this incision a pustule, taken carefully from the body of another child,” he wrote. “This pustule produces the same effect in the arm it is laid in as yeast in a piece of dough…”
Voltaire goes on to argue that the French should be more open-minded toward the idea of inoculation, which was already standard practice in England to prevent smallpox. He continues: “I am informed that the Chinese have practiced inoculation these hundred years, a circumstance that argues very much in its favor, since they are thought to be the wisest and best governed people in the world. The Chinese, indeed, do not communicate this distemper by inoculation, but at the nose, in the same manner as we take snuff. This is a more agreeable way, but then it produces the like effects; and proves at the same time that had inoculation been practiced in France it would have saved the lives of thousands.”
1777. Because smallpox was such a destructive disease, even George Washington ordered mandatory inoculation for troops who hadn’t survived smallpox before.
1796. Enter Edward Jenner, an English physician and scientist who would later become known as the “father of immunology” due to his pioneering vaccination work. In the 1760s, Jenner learned that in the countryside, dairy workers would often be infected with cowpox — a similar, but much milder, disease than smallpox which is in the same Orthopox virus family — and because of this, they would never be infected with smallpox. Jenner decided to experiment with this phenomenon, and he took pus from a person infected with cowpox then rubbed it into the scratched arm of an 8-year-old boy. The boy never caught smallpox. This ushered in a new, safer method of inoculation.

1840. During the next decades, Jenner’s method of cowpox inoculation — which was soon dubbed “vaccination” (from Variolae vaccinae, meaning smallpox of the cow) — grew more popular and soon overtook that of smallpox inoculation, as the former was much safer. Smallpox inoculation then simply became known as variolation, referring to smallpox (Variola). For some time, both vaccination and variolation were available, but governments soon began arguing that only vaccination was safe. In 1840, England banned variolation.

1880s. Like many scientific breakthroughs, the development of a vaccine for chicken cholera and anthrax happened somewhat accidentally. French chemist and microbiologist Louis Pasteur was working at the time on learning more about chicken or fowl cholera. Pasteur usually introduced lab cultures of the bacteria into his lab chickens, resulting in their deaths. But once, while on vacation, he left cultures of the bacteria lying around idly. Upon his return, he exposed the chicken to the bacteria, without knowing the bacteria were weakened or dead. The chickens didn’t die from the disease like before. Even when he injected the same chickens with a potent bacterial culture afterwards, they were protected from disease. Pasteur realized this was a form of inoculation against fowl cholera, and he used the same method for an anthrax vaccine.
1881. This was a seminal year for vaccine development. Pasteur staged a public demonstration in which he inoculated 24 sheep, one goat, and six cows against anthrax, and left another group of farm animals unvaccinated. Several weeks later, he exposed them all to anthrax bacilli, then allowed the crowd to regather two days later. All of the vaccinated animals survived, in comparison to the control group which did not survive. Within a few years, Pasteur developed a rabies vaccine as well using the same inoculation method.
1920s . While Jenner and Pasteur were the two main pioneers of vaccination in their early days, by the 1920s many more vaccines had been developed and become widely available, including diphtheria, tetanus, whooping cough, and tuberculosis (TB), according to the NHS.
1950s. Researchers had been attempting to develop a vaccine for polio — a devastating disease that often left children paralyzed or dead — since the 1930’s, but the major breakthroughs didn’t occur until the 50’s. During this time, the U.S. had been experiencing a polio epidemic, making the need for a vaccine that much more crucial.
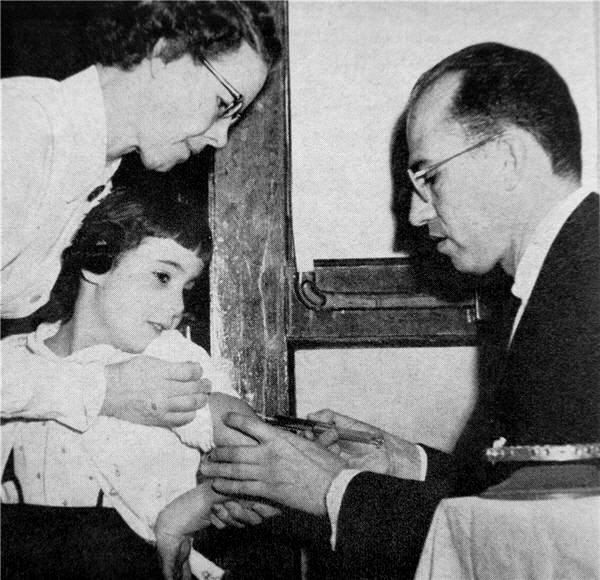
In 1952, Jonas Salk and his research team at the University of Pittsburgh developed the first effective polio vaccines. Several large studies showed the vaccine to be largely effective against several different types of the poliovirus. Three years later, in 1955, a huge children’s polio vaccination campaign was launched, resulting in a dramatic decrease in polio cases in subsequent years. The cases fell from 35,000 in 1953 to 5,600 in 1957; and by 1961, there were only 161 cases in the U.S.
1960s-70s. The vaccines for meningococcus and pneumococcus are developed.
1980. Smallpox is eradicated from the entire globe; this landmark is considered one of the most incredible achievements in medicine.
1994. Polio is declared eliminated from the Americas. In 2002, it was eliminated from Europe (today, only Pakistan and Afghanistan continue to have polio cases).

1998. This year marked the emergence of a controversial paper published in The Lancet. Andrew Wakefield, a British researcher at the time, linked the MMR vaccine with autism spectrum disorders in the paper. Later, the paper was found to be fraudulent, and it emerged that Wakefield had been funded by opponents of vaccine manufacturers.
However, the damage had already been done. In the U.K., vaccination rates fell from 92 percent to 80 percent in the years after the study, which gave birth to the Anti-Vaxxer movement that is once again gaining traction in the U.S.
2006. The first HPV vaccine is developed.
2014. The CDC reports the highest number of measles cases in the U.S. since measles was declared eliminated in 2000.
Currently, though we’ve come a long way in fighting infectious diseases that were once widespread, researchers are still working on vaccines that could prevent herpes simplex, malaria, gonorrhea, HIV, ebola, and Zika. On top of that, studies have shown that Anti-Vaxxer sentiment around the U.S. has increased in recent years, contributing to the parallel drop in vaccination rates. Indeed, anti-vaccination beliefs were common hundreds of years before, when inoculation was still considered dangerous; but since then studies have repeatedly shown that vaccines do not cause autism and they are completely safe.
If we stopped immunizing children against preventable diseases, the chance of a serious outbreak occurring would increase. A recent study found that a large chunk of measles and whooping cough cases in the U.S. are made up of Anti-Vaxxers, or people who believe vaccination is harmful or unnecessary. These same people are the ones who drive the return of infectious diseases that had once been eradicated. The recent measles outbreak at Disneyland, for example, emphasizes the importance of vaccinating all kids.
Published by Medicaldaily.com



























