New Breast Cancer Screening Guidelines From American Cancer Society Push Mammogram Age From 40 To 45
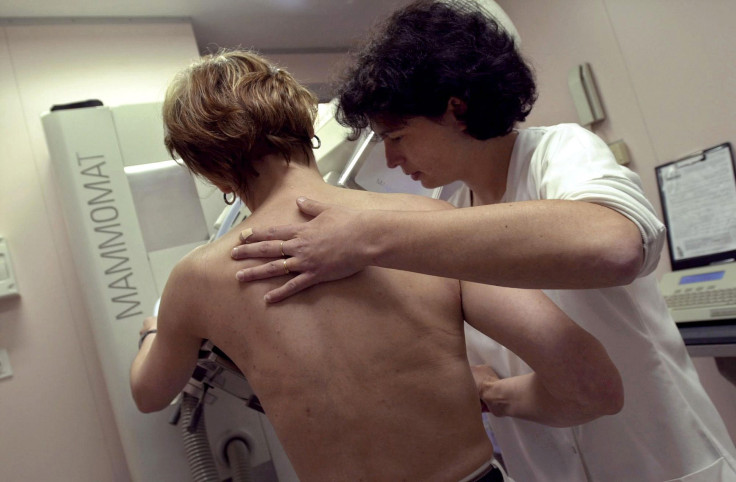
The American Cancer Society’s (ACS) age recommendation for early breast cancer detection — essentially the earliest age a woman should get her first mammogram — has been pushed back from age 40 to 45. The new guidelines were published Tuesday in JAMA.
“Since the last ACS breast cancer screening update for average-risk women was published in 2003, new evidence has accumulated from long-term follow-up of the randomized controlled trials (RCTs) and observational studies of organized, population-based screening (service screening) programs,” the ACS wrote. “In addition, there is now greater emphasis on estimating harms associated with screening.” So the ACS thought it best to organize an interdisciplinary development group to update the 2003 guidelines.
A group of clinicians, biostatisticians, epidemiologists, an economist, and patient representatives were tasked with answering three key questions:
- What are the relative benefits, limitations, and harms associated with mammography screening compared with no screening in average-risk women 40 years and older, and how do they vary by age, screening interval, and prior screening history?
- Among average-risk women who are screened with mammography, what are the relative benefits, limitations, and harms associated with annual, biennial, triennial, or other screening interval, and how do they vary by age?
- What are the benefits, limitations, and harms associated with clinical breast examination (CBE) among average-risk women 20 years and older compared with no CBE, and how do they vary by age, interval, and participation rates in mammography screening?
In addition to answering these groups, ACS’s group of experts evaluated the available methods and the strength of current screening recommendations. This group then selected the Duke University Evidence Synthesis Group to conduct an independent systematic evidence review of the breast cancer screening literature after a response to a request for proposals. The Breast Cancer Surveillance Consortium was also approached to update previously published analysis related to screening interval — annual or biennial — and outcomes.
After all was said and done, the group’s official recommendations were as follows: Women with an average risk of breast cancer should undergo regular screening mammography starting at age 45; women aged 45 to 54 years should be screened annually; and women aged 55 years and older should transition to biennial screening or have the opportunity to continue screening annually.
Drs. Nancy L. Keating and Lydia E. Pace wrote in an accompanying editorial that “several aspects of this new guideline will be particularly striking to patients, clinicians, and others involved in health care,” from the “more conservative starting age” to “the recommendation against routine screening CBE.” Yet, they added that these new guidelines are the result of a “thorough evidence review” and “several methodological decisions that led to these novel recommendations.”
Keating and Pace admitted women and clinicians following new ACS guidelines may find it confusing to transition from no screening when younger than 45 years to annual screening from ages 45 to 54 years, and then to biennial screening. But, for what it’s worth, the guidelines “are now more consistent.” And they agree that for average-risk women younger than 45, the harms of mammography “likely outweigh the benefits.”
That said, the evidence needed to help women make decisions related to breast health “remains incomplete,” Keating and Pace said. Instead, they said women should be supported in estimating and understanding their personal risk for developing breast cancer in order to reach informed decisions with their clinician.
“The future of breast cancer screening is likely to entail a more personalized understanding of breast cancer risk, one that incorporates both published risk assessment tools using combinations of known risk factors with newer techniques such as genomics,” Keating and Pace concluded. “If women who are at higher risk of aggressive breast cancer could be more accurately identified, for example, it would be possible to more definitively identify those women who are most likely to benefit from earlier and more frequent breast cancer screening and less likely to experience the related harms.”
Source: Smith RA et al. Breast Cancer Screening for Women at Average Risk 2015 Guideline Update From the American Cancer Society. JAMA. 2015.
Published by Medicaldaily.com



























