Psoriasis Skin Management for Plaque Psoriasis with Biologic Injections and Skin Barrier Repair
Psoriasis skin management is an ongoing strategy that combines topical therapy, light therapy, systemic medications, and sometimes biologic injections to keep plaque psoriasis under control while supporting overall skin health.
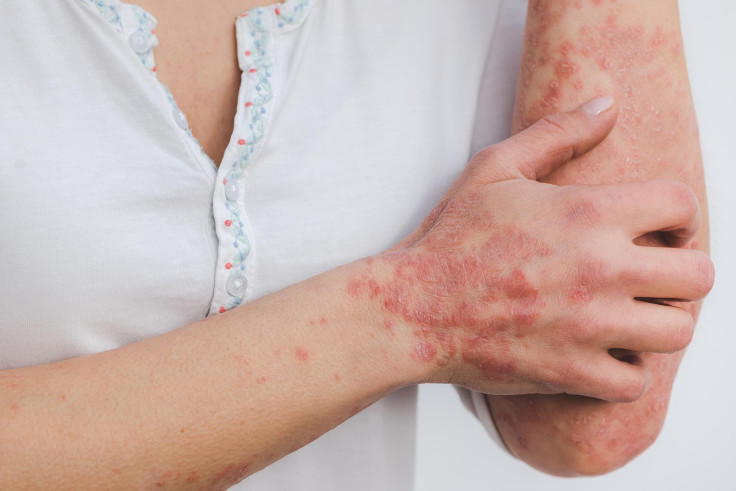
Plaque psoriasis is the most common form and appears as raised, red, scaly patches caused by an overactive immune response that speeds up skin cell growth. Because the condition affects both the skin surface and deeper immune pathways, treatment often layers different approaches rather than relying on a single option.
Psoriasis Skin Management and Plaque Psoriasis
A central issue in plaque psoriasis is disruption of the skin barrier. When this barrier is weakened, the skin loses moisture more easily and becomes more prone to irritation, cracking, and infection.
Skin barrier repair through daily use of emollients, gentle cleansers, and avoidance of irritants is therefore a key part of psoriasis skin management. This supportive care pairs with medical treatments to improve comfort, help medications penetrate better, and potentially reduce flare frequency.
First-Line Topical Treatments
Topical therapy is typically the first-line treatment for mild or localized plaque psoriasis. These medications are applied directly to affected skin to reduce inflammation, slow excessive cell growth, and ease symptoms like redness, scaling, and itch.
Common options include corticosteroid creams or ointments and vitamin D analogues, sometimes combined in a single product for added benefit.
Stronger corticosteroids may be used for thick plaques on areas like the elbows or knees, while low-potency steroids or non-steroidal topicals are preferred for sensitive locations such as the face or skin folds.
Role of Skin Barrier Repair with Topicals
Consistent use of moisturizers and emollients works alongside these prescription topicals to support skin barrier repair. Thick, fragrance-free moisturizers soften plaques, decrease scaling, and help the outer layer of skin hold onto water.
For many people, this daily step becomes a stable foundation of psoriasis skin management that continues even when other treatments change over time. When plaque psoriasis is more widespread or does not respond adequately to topical therapy, additional options are usually considered.
When Light Therapy Is Used
Light therapy, or phototherapy, is often recommended when plaque psoriasis is moderate or not well controlled with topicals alone. In medical settings, carefully measured doses of ultraviolet light are directed at affected skin to slow rapid skin cell turnover and reduce inflammation, according to the World Health Organization.
Narrowband UVB is commonly used because it focuses on a helpful wavelength while limiting some of the broader UV range. Treatment typically involves several sessions per week over a number of weeks, with doses adjusted based on response and side effects.
Benefits and Risks of Phototherapy
While many people see noticeable improvement with phototherapy, risks must be considered. Short-term side effects can include redness, dryness, and sunburn-like reactions, while long-term cumulative exposure may increase the risk of photoaging and certain skin cancers.
Because of this, clinicians track total exposure and may use light therapy as one part of a broader psoriasis skin management plan rather than as a permanent, high-frequency treatment.
When Systemic Meds Are Considered
Systemic medications are used when plaque psoriasis is moderate to severe, covers large areas, or is associated with joint symptoms.
These drugs act throughout the body to reduce immune-driven inflammation, often improving skin plaques and related symptoms together. They are usually introduced when topical therapy and light therapy are not sufficient to keep disease activity under control.
Types of Systemic Treatments
Traditional systemic options include methotrexate, ciclosporin, and acitretin, all of which require regular monitoring because of potential effects on organs such as the liver and kidneys, as per the Centers for Disease Control and Prevention.
Newer oral agents that target specific immune pathways have expanded choices for people who prefer pills or who are not good candidates for injections. In every case, the decision to start systemic treatment is individualized, taking into account disease severity, other medical conditions, and personal treatment goals.
How Biologic Injections Work
Biologic injections are a major development in systemic treatment for plaque psoriasis. These therapies target specific molecules, such as TNF, IL‑17, or IL‑23, that drive inflammation in psoriasis.
By focusing on these pathways, biologic injections can offer strong and sustained improvements in skin clearance for many individuals whose disease has not responded well to older therapies.
They are usually given as periodic injections, often starting with a loading phase followed by regular maintenance doses that can sometimes be spaced weeks apart.
Safety and Long-Term Use of Biologics
Because biologic injections alter immune function, careful screening and follow-up are important parts of psoriasis skin management. Before treatment, individuals are typically checked for underlying infections and other health concerns.
During treatment, clinicians monitor for infection risk and other potential side effects while balancing benefits against any emerging issues. Biologic injections can be combined with topical therapy and supportive skin barrier repair measures to fine-tune control.
Long-Term Psoriasis Skin Management for Better Control
For most people, long-term psoriasis skin management involves a personalized mix of therapies rather than a fixed, single regimen. Topical treatments and moisturizers are often constant companions, while light therapy, systemic medications, or biologic injections are added or adjusted depending on disease severity and life circumstances.
By focusing on plaque psoriasis control, consistent skin barrier repair, and steady communication with a healthcare professional, many individuals can achieve better symptom control and maintain more comfortable, resilient skin over time.
Frequently Asked Questions
1. Can psoriasis skin management help reduce itch without increasing medication?
Yes. Regular use of emollients, gentle cleansers, and avoiding hot showers or harsh soaps can reduce itch by supporting skin barrier repair, even without changing prescription treatments.
2. Is it safe to stop biologic injections once plaque psoriasis improves?
Stopping biologic injections is possible, but flares are common. Any change should be planned with a dermatologist, who may suggest tapering or switching to a different long-term strategy.
3. Can light therapy and topical treatments be used at the same time?
Yes. Phototherapy is often combined with topical treatments and moisturizers, which can improve comfort, support the skin barrier, and sometimes enhance overall response.
4. Do systemic psoriasis medications help with fatigue and joint pain too?
They can. Because systemic and biologic treatments act on whole‑body inflammation, some people notice improvements in fatigue and joint symptoms along with better skin control.
Published by Medicaldaily.com