World Sickle Cell Day 2015: How Rare Disease Awareness Leads To Quality Care, Treatment
Rare diseases, like sickle-cell disease (SCD), often don’t get the attention they deserve. The non-profit organization Global Genes found an estimated 95 percent of rare diseases don’t have a single FDA-approved drug treatment — there are only 400 treatments approved to treat some 7,000 rare diseases believed to be affecting people today. It's clearly not enough.
But with more awareness and education, Global Genes reported, doctors, patients, and their families have improved access to treatments and medical representation. So while Feb. 28 (depending on if it’s a leap year) recognizes rare diseases worldwide, June 19 specifically focuses on SCD. The United Nations created the awareness campaign back in 2006.
“[SCD] is an extremely debilitating medical condition. It is characterized by chronic pain with frequent bouts of acute severe pain that requires large amounts of narcotics that often provide incomplete relief,” said Dr. Yutaka Niihara, chief scientific officer of Emmaus Medical and professor of medicine at the David Geffen School of Medicine at UCLA, in an article last year. “It is also marked by social stigma that makes others, including medical professionals, view sickle cell patients as ‘drug seekers’ due to their need for large amounts of pain medication.”
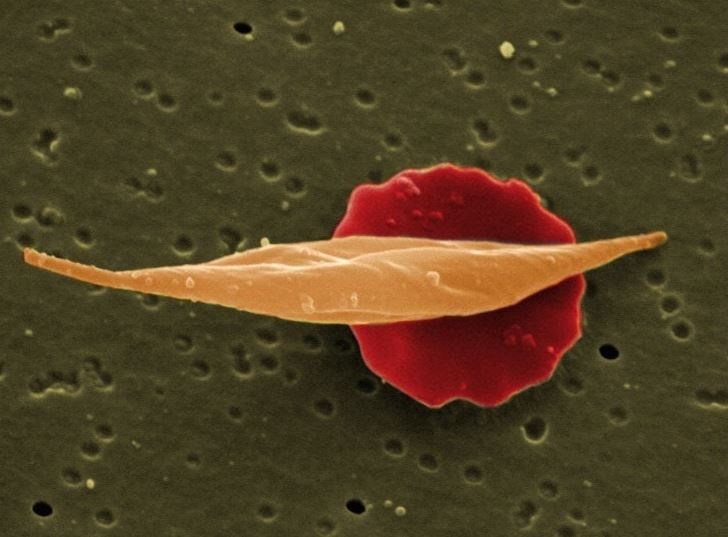
Essentially patients who inherit SCD (it’s a hereditary disease) have poorly oxygenated red blood cells in the shape of a C-shaped farm tool called a “sickle.” Patients’ cells are hard, sticky, and sometimes travel backwards, according to the Centers for Disease Control and Prevention (CDC). Cells get stuck this way and clog blood flow, leading to “pain and other serious problems such as infection, acute chest syndrome, and stroke.”
“Any day without pain is a good day,” Shakir, an activist for SCD awareness and research, told Global Genes. Niihara added patients “have an annual average of three episodes of severe pain that requires hospitalization and narcotics.” But unfortunately, he said many people, and that includes medical providers, don’t understand their pain and undertreat them, if at all.
“[SCD] patients’ pain is real and is triggered by damage to major parts of their bodies, including the heart, lungs, kidneys, and brain,” Niihara said. “Also, they are very susceptible to infection, which can be life threatening. These organ damage-induced bouts of pain and infectious episodes are two causes of mortality at a very young age.”

Today, the CDC reports an estimated 90,000 to 100,000 people in the U.S. are affected by the disease, mainly blacks or African-Americans;” Hispanics come in second. Worldwide, however, SCD is prevalent in sub-Saharan Africa, South America, Central America, Saudi Arabia, India, Turkey, Greece, and Italy.
The life span of someone with SCD is about 40 years if they live in the U.S. Niihara explained that in underdeveloped countries, where there’s limited access to medical care, 90 percent of patients won’t live past age 5.
Relief, especially for SCD-related pain, is limited. Some experts recommend patients drink plenty of water, keep their body temperature regulated, and avoid high altitudes and low oxygen levels. For more severe cases, the CDC says hydroxyurea is an option, a medication designed to reduce the number of painful episodes. However, the medication boasts serious side-effects and anyone taking it should do so under a doctor's supervision.
Even the multiple blood transfusions that keep red blood cell levels up pose health risks with increased transfusions overloading the body with iron. Too much iron can lead to liver, heart, and pancreas damage, the CDC found. The only source of long-term relief for SCD patients is either bone marrow or stem cell transplants, which on their own are very risk.
Being vocal about the realities of living with SCD has a positive domino effect.
“By telling a story, you can help shed light on a condition’s symptoms, prognosis, and other details for those still searching for the correct diagnosis or for someone who knows their disease firsthand,” Global Genes found. “Medical terminology and data, though important, can obscure what it means to live with a disease and make it difficult for most people to relate. Personal stories, though, frame our individual rare experiences in a way that lets others connect.”
That said, patients are hesitant to come forward with their stories. In the Mental Health Channel’s video “THE COMMON GOOD: Above The Crisis,” patients admit they don’t want to be the person to say, “Hey, you know I have sickle cell… but in essence that’s our problem, we keep it to ourselves, so that’s kind of why we don’t have a community.” Encouraging others to speak up chips away at the stigma regarding SCD, inviting others to address the day-to-day challenges of SCD, especially those pertaining to mental health.
“It’s so easy to be consumed by sadness when you’re this sick,” LeDarrin, who has SCD and directed MHC’s video, said. “You have to make a conscious decision not to be. And I just decide every day to have some joy.”
You can watch the video in full below:
THE COMMON GOOD: Above The Crisis from mental health channel on Vimeo.
Published by Medicaldaily.com



























