Is C-Section Popularity The Result Of Doctors Wanting More Money? Obstetricians Paid More For Cesarean Births
Approximately one in three babies in the United States are now delivered by Cesarean section, a surgical procedure commonly known as a C-section. New research conducted by health care economists Erin Johnson and M. Marit Rehavi suggests that monetary incentives influence how obstetricians advise pregnant women about delivery, especially when it comes to deciding whether to have a C-section.
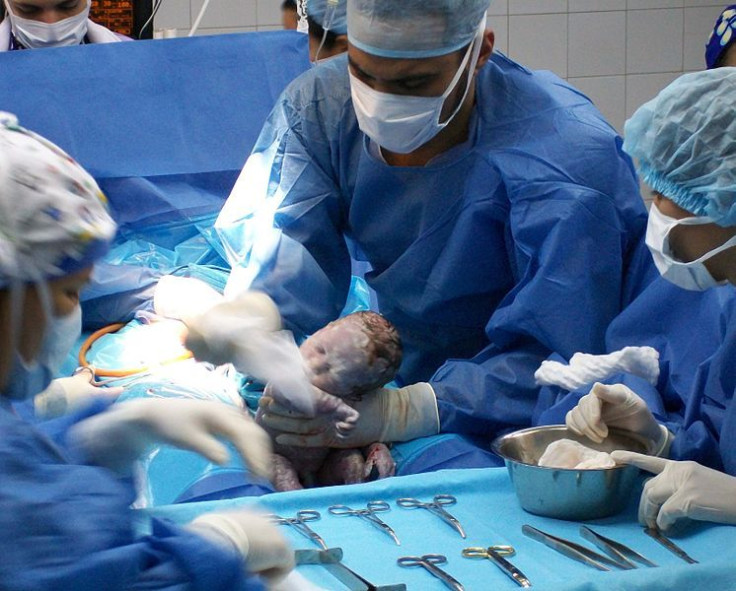
A C-section involves a surgical procedure in lieu of vaginal birth. During a C-section delivery, a doctor makes an incision in the mother’s abdomen and uterus through which the baby is pulled.
According to Family Education, vaginal deliveries are considered safer than C-sections. An invasive surgical procedure, Cesarean sections carry the risk of complications and take longer to recover from compared to vaginal birth. In most cases, C-section should only be an option under extreme health conditions for either the mother or the baby. Some maternal indications for C-section include risk for disease transmission, inability to labor, and having a pelvis too small to allow a baby to pass through. Fetal indications for C-sections include umbilical cord complications, fetal distress, and multiple babies (i.e. twins).
So why are so many healthy mothers and babies opting for C-sections, even though it seems to be an option left for those families in dire emergency? The answer may lie in obstetricians' pocketbooks.
Based on Johnson and Rehavi’s research, obstetricians may get paid an extra few hundred dollars to perform a Cesarean than a natural delivery. Though the amount may not seem like a lot, for doctors who deliver five to 10 babies a week, that number adds up pretty quickly. Interestingly, doctors who purportedly performed more C-sections than necessary opted to have natural vaginal births when it came to their own pregnancies.
"We found that doctors are about 10 percent less likely to get C-sections," said Johnson. "So obstetricians appear to be treating their physician patients differently than [they treat] their non-physician patients."
"The idea is that physicians have medical knowledge," Johnson told NPR. "If the obstetrician is deviating from the best treatment because of their own financial incentive, the patient [who is a] doctor would be able to push back against the obstetrician. But that might not be the case for non-doctors because they simply do not have the medical knowledge to know whether or not this C-section is the appropriate [method of delivery] for them."
Doctors aren't necessarily consciously suggesting C-sections more often; the research teams suggests obstetricians may be doing so subconsciously. Financial incentives have perverse effects on the mind.
But the financial incentive to perform C-sections is likely to stay. So to help curb the over-use of surgical births, the study authors suggest that pregnant woen should be educated about the safety risks of C-section as well as the health benefits associated with vaginal birth.
Published by Medicaldaily.com



























