Hospital CEO Pay Not Based On Quality Of Care Or Mortality Rates: Urban Hospitals With High Patient Satisfaction Pay Most
In many organizations, a chief executive officer is paid based on performance and often must reach certain milestones in order to achieve a certain pay bonus, but what is at stake when compensating a CEO of a hospital?
A team of researchers asked exactly this question in a recent study of nonprofit hospitals in the U.S. and discovered that quality of care, community benefit, and most surprisingly, actual patient outcomes did not seem to matter nearly as much as two other factors. When it came time to signing off on a CEO’s salary, advanced technologies and high ratings of patient (customer) satisfaction seemed to trump all other factors.
Is This Just Business As Usual or Medicine?
The researchers, who are associated with Harvard School of Public Health, Brigham and Women’s Hospital, and Veteran’s Affairs Boston Healthcare System, collected data from tax returns, hospital surveys, and performance reports and then used linear regression to identify characteristics associated with CEO pay. For this observational study, ‘participants’ included 1,877 CEOs at 2,681 private, nonprofit U.S. hospitals. The team of researchers determined that CEOs had a mean compensation of $595,781 (median, $404,938) in 2009.
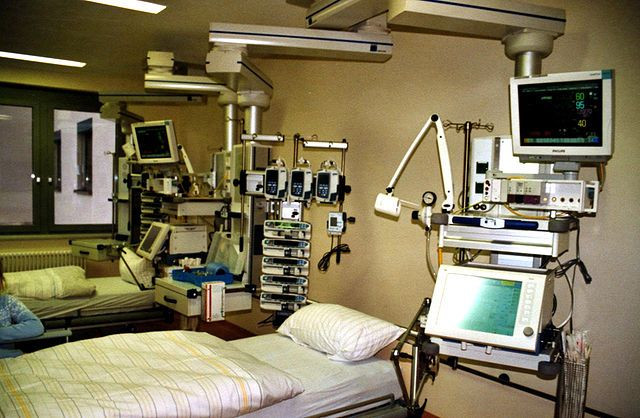
Although the team found that CEO pay was linked to the number of hospital beds overseen ($550 for each additional bed), whether a facility qualified as a teaching hospital, and location — urban trumped suburban or rural locations — these were not the key factors when it came to pay. Instead, what seemed to matter most was whether a hospital had high levels of advanced technologic capabilities; CEOs at such hospitals received $135,862 more in compensation than those at hospitals with low levels of technology. And, hospitals that showed high performance on patient satisfaction paid $51,706 more to their CEOs than those with lower numbers for that criterion.
Unusually, the team found no association between CEO compensation and other hospital performance factors that many people would find most significant, such as mortality rates, readmission rates, occupancy rates, process quality performance, overall hospital capitalization, or any measure of community benefit.
"I think we were a little disappointed," Dr. Ashish Jha, one of the study's authors, told Reuters. "I was hoping I'd see even some modest relationship with quality performance."
Despite the general results, the researchers emphasize that executive paychecks at hospitals varied widely. Those executives who fell within the highest 10 percent category earned close to $1.7 million per year and were charged with oversight of generally large, teaching hospitals in cities. CEOs with salaries and bonuses in the lowest 10 percent earned, on average, just $118,000 a year. These more humble executives mostly worked at small, non-teaching hospitals in rural areas.
What may come as a surprise to those outside the field of medicine is that another article, which appears alongside the study in JAMA Internal Medicine, discusses how physicians may also have become much too concerned with 'customer' satisfaction.
Not Just Hospital CEOs, But Doctors, Too
In a “Viewpoint” article, Dr. C. Bree Johnston of the PeaceHealth Medical System examines the same trend that has emerged in the area of physician reimbursement. Noting that high patient satisfaction scores are increasingly used as a metric when determining a doctor’s compensation, Johnston wonders if such scores are effective for assessing quality of care. Within the article, she notes that higher patient satisfaction scores may be associated with higher hospital admission rates, higher expenditures for both medical care and prescription drugs, and even increased rates of mortality.
“Oncologists who are more optimistic---even if they give patients unrealistic information---are rated more highly than their more realistic colleagues,” Johnston wrote.
A professional confession reveals the direct and nearly immediate effect on a physician’s behavior when patient satisfaction becomes primary in compensation considerations. Johnston provides the example of a colleague who no longer confronts patients on their drug abuse or gives them bad news because it might lower satisfaction scores. Who would want to give bad news under circumstances that are stressful, take extra time, cause people to dislike you, and “will lower your income”? Johnston wondered.
Although understandable to some extent, isn’t the maxim ‘do no harm’ the first rule of medical ethics? Most of us would consider a doctor who provides false information or fails to deliver bad news as performing an ‘act of harm.’ As the rest of us understand, ethics have always and will always impact paychecks in every field — why should doctors be exempt?
Sources: Joynt KE, Le ST, Orav EJ, Jha AK. Compensation of Chief Executive Officers at Nonprofit US Hospitals. JAMA Internal Medicine. 2013.
Johnston CB. Patient Satisfaction and Its Discontents. JAMA Internal Medicine. 2013.
Published by Medicaldaily.com



























