Refugees In America’s Healthcare System: How Refugee Families Get The Care They Need To Build New Lives

In a small duplex on a quiet street in Cleveland, Ohio, an Iraqi family of five is beginning its new life in America.
The Al Alawi family has been in the U.S. since mid-December. Khalid is a father of three and the grandfather of Rema, a quiet 3-year-old. Shahrazad, Khalid’s wife, speaks with warmth and intelligence, and when I visited on a January morning, she offered me cookies and hot chocolate almost immediately. She introduced me to Ayad, her 35-year-old son with autism, who is unable to communicate.
They’re here to give their children and grandchildren a new chance at a fulfilling, educated life. They also hope to secure the help for Ayad that they could never have found in their home country.
“Doctors didn’t know what to do,” said Shahrazad, who worked as a dentist in Iraq. “Even doctors didn’t know the word autism. There really weren’t any psychologists there. They said that America was the best place for this kind of thing.”

Throughout the hour that I spoke with the family, Ayad sat quietly in his chair; he stared at the wall in front of him, and never said a thing. But he was always smiling. His parents explained that he doesn’t talk unless he’s speaking with his younger brother, who is still in Jordan but trying to leave for America. Only with his brother does Ayad open up and begin to communicate in Arabic. Every day, his family washes Ayad, dresses him, and asks him to do simple household tasks to move around — otherwise he’d simply sit in a corner. His actions are limited, and whenever he’s exposed to change he seems to regress.
“He can’t differentiate between right or wrong,” Shahrazad said. “You have to follow him everywhere, even across the road.” Her eyes filled with tears.
“We pray to God to find a way to help him,” Khalid added.
The Al Alawis are among the thousands of refugees who resettle in the U.S. every year in an effort to escape the wars and humanitarian crises in their home region. For some, resettling is also an opportunity to find proper medical care. Not all refugees have a diagnosis like Ayad, but a large amount of them have special medical and mental health needs.
Refugees are eligible for Medicaid under the Affordable Care Act, but they still face plenty of obstacles to receiving proper care. In cities across the U.S., refugee agencies work locally to remove some of these barriers to health care. Former refugees help newly-arrived ones to get their feet on the ground, but they also hope to go beyond the basics, offering specialized mental health services and programs for survivors of torture to heal the wounds of war.

How To Ride the Bus
There are some 19.5 million United Nations-registered refugees displaced due to conflict or persecution throughout the world, according to June 2015 data from the UN High Commissioner for Refugees (UNHCR). Only 1 percent end up getting relocated to a developed third country; the rest remain in their crisis-ridden countries (like Syria or Iraq) or in refugee camps in host countries like Jordan. This is mainly due to the rigorous, lengthy, screening and interviewing process they have to go through.
“There are background checks… and the vetting process continues from the first step until their arrival in the U.S.,” Will Haney, a spokesperson for Church World Service in New York City, told Medical Daily . “Refugees are the most vetted population entering the U.S. If [officials aren’t 100 percent] certain, those refugees are not going to be coming to the U.S.”
For the past several years, America has been accepting 70,000 refugees annually, most of whom are from Africa, Asia, and the Middle East, though many are also from the former Soviet Union (such as Ukraine and Russia). In 2015, Ohio accepted 316 refugees from Iraq and Afghanistan, 78 from Syria, and hundreds of others from other countries — including Bhutan, the former Soviet Union, the Democratic Republic of Congo, and Somalia. After the U.S. accepts a refugee, the federal government works with nine refugee agencies who then relay the refugee’s information to other, smaller resettlement agencies scattered throughout the country.
“All of the little things that we take for granted, the resettlement agency helps [the refugees] with,” Bill Swersey, communications director at New York City-based HIAS (formerly the Hebrew Immigrant Aid Society), told Medical Daily. “The goal is to get them up on their own two feet in a relatively short period of time.”
Health care is key. In the U.S., it can be difficult for the average person to keep up with a quickly changing and evolving health care system. Refugees, many of whom have never experienced a Western health care system, often face language barriers and usually do not have their own transportation.
In Ohio, Us Together is one of the smaller refugee agencies that provides services for newly arrived refugees. Founded and run by former refugees, the agency helps remove hurdles to health care by educating refugees about pharmaceuticals, providing families with a mentor, and offering transportation services to the doctor’s office.
One example of Us Together’s work is a newly established pharmacy program in Columbus. Once or twice a month, refugees gather for a two-hour class where they learn about how to get and fill prescriptions at pharmacies. Workers also sit down with refugees to teach them about the transportation system in their city, showing them how to ride the bus to the hospital or doctor’s office.
The goal for all refugees, explained Us Together director and co-founder Nadia Kasvin, is to ultimately have a job within four to six months of their arrival to the U.S. “We need to address any mental and medical issues they might have, and remove those barriers to finding a job,” Kasvin told Medical Daily.
For the Al Alawi family, that means finding help for Ayad — so that both parents and Ayad’s sister will be able to work without having to care for him 24/7. Finding work is a matter of survival for resettled refugees; it defines the difference between a new life and a spiral into another crisis.

Khalid, who has a Masters degree in engineering and was a professor in Libya and Jordan for several years, will have to completely re-start here in the U.S. “I would love to take a part-time job in teaching,” Khalid said. “When I found this teaching job in Libya, I found it very touching. The years flew by. Teaching is important to me, it’s a lovable job.” But without U.S. credentials, Khalid will be more likely to have to take a more menial job, like working at a restaurant or store.
And before Ayad can be sent to an autism specialist or community groups, the Al Alawi family must first go through the government-mandated health screenings that are necessary upon the first month of arrival.

Stealing Their Blood
On a Monday morning at Neighborhood Family Practice (NFP) in Cleveland, the waiting room was filled with the chatter of foreign languages — Swahili, Spanish, Arabic, Nepali. Nearly everyone is a newly-arrived refugee, escaping either a recent conflict or 20 stalled years in a refugee camp, and waiting to undergo their first health screening in America.
“It’s like the UN in here on Mondays,” said Jamie Bullus, NFP’s Refugee Services Program Coordinator.
These refugees have all already undergone initial health screenings abroad; according to the CDC, if a refugee has a Class A condition — active or infectious tuberculosis (TB), leprosy, untreated syphilis or gonorrhea, or mental health issues that are considered dangerous — they don’t make it to the next step, and can’t enter the U.S. Class B conditions include inactive or latent TB, treated STDs, or pregnancy: things that have to be cared for before they get to the next step. Refugees with a history of suicide or crime are disqualified, as they may pose a threat upon entering.
Then, on arrival each refugee goes through another standard government-regulated health screening . “The overseas medical exam is an exam of exclusion,” said Bullus. “Every exam up to this point is why you can’t go to the U.S. Now that they’re here, if there’s anything wrong with them, they can begin to open up.” Each year, NFP, screens over 600 refugees upon their arrival in the U.S., and 70 percent of these refugees return to NFP for primary care.
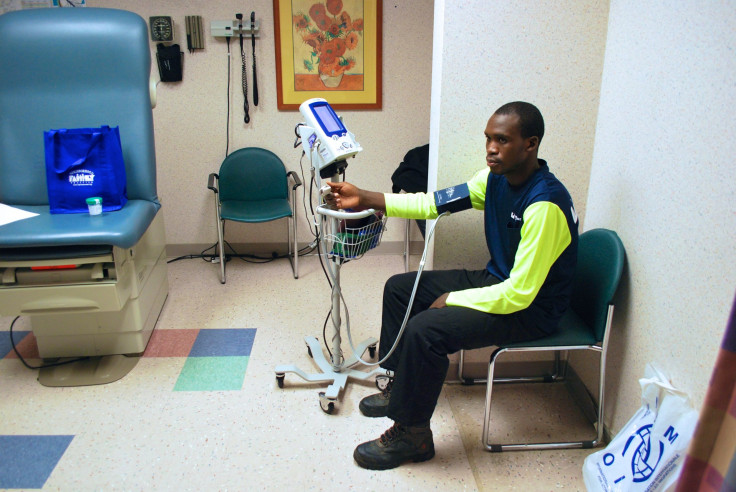
Izabayo Nsabiyeze sat in a small room as a medical assistant asked him about his medical and family history. Nsabiyeze is Congolese, but before coming to America he lived in a refugee camp in Uganda for 18 years. He spoke broken English, but felt far more comfortable speaking Swahili, so another former Congolese refugee acted as an interpreter. The medical assistant went through a checklist of standard questions: How many siblings do you have? Have you had any aches or pains? Did you experience torture or trauma while you were living abroad? There are stool and urine samples, vision and weight measurements, a flu vaccine, and blood tests.
The refugees will return to the medical center a week later for a second part of the screening process, in which they’ll be asked to complete a mental health survey, typically printed out in their native language. Because most refugees come from countries that have no mental health system in place and where the idea of seeking mental health counselling is stigmatized or completely unheard of, the survey words symptoms as something physical: “feeling faint, dizzy, weak, restless,” or “crying easily, feeling numb when reminded of the trauma.”
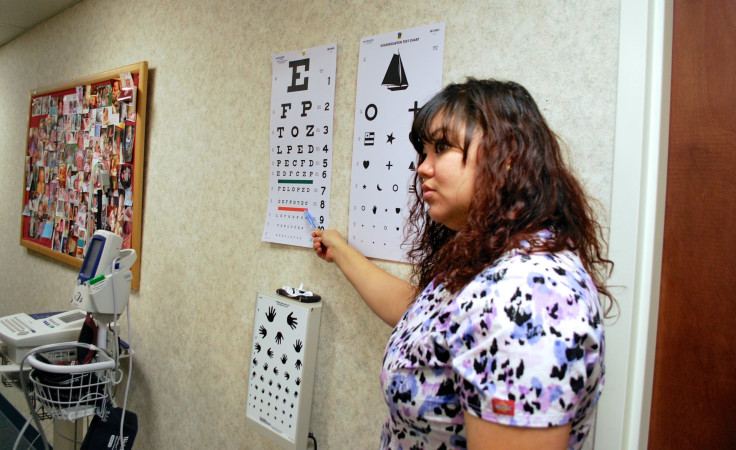
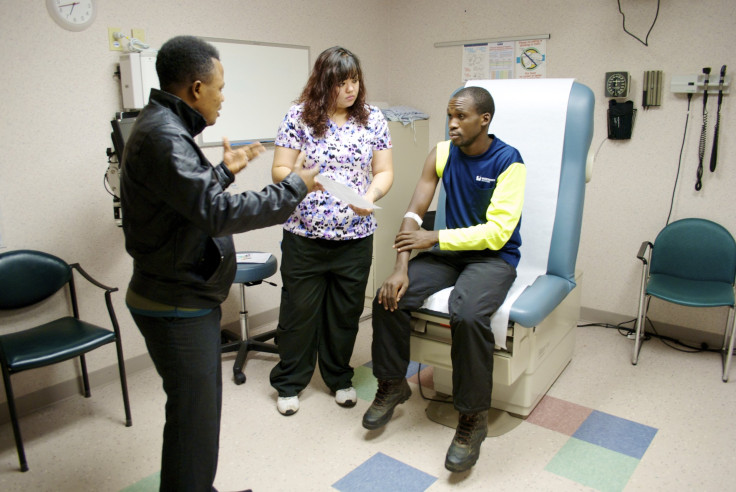
After getting vials of his blood drawn, Nsabiyeze returned to the room looking a little bewildered. He asked the medical assistant why so much blood was taken from him: “What are they going to do with all of my blood?”
As confusion over medical practice is common, it’s NFP’s job to help the refugees understand the Western viewpoint on medicine a little better. “A lot of times it just comes down to explaining what it’s for and taking that extra minute,” Bullus said. “We have groups who don’t want their blood taken; they think we’re stealing it. … Some cultures don’t think they should have to take medicine every day, as they think it means they’re very sick. That’s why every visit is a little bit of a health education.”
While educating patients, NFP doctors must also be aware of each culture’s health quirks to better treat them. Bullus sent emails to the staff during Ramadan to remind nurses and physicians that their Muslim patients’ blood sugar levels may be off that week. And NFP doctors deal with chronic conditions rarely seen in the U.S., like malaria, intestinal parasites, lead poisoning, and anemia, which are incredibly common among refugee populations.
“We’re trying to practice global health in Cleveland,” Bullus said. “You don’t expect to see malaria in Cleveland, but our providers do.”
“They Create Their Own Crisis”
The average American hasn’t survived war crimes or torture, or lived in a refugee camp for 25 years. But even among Americans, getting access to mental health care isn’t always easy due to stigma , cost, or a shortage of mental health care practitioners. So when it comes to refugees, most of whom have survived trauma in one way or another, helping them get access to health care is a priority for refugee agencies.
Research has shown that Syrian refugees living in camps are more likely to have depression, anxiety, post-traumatic stress disorder (PTSD), and other mental health problems than those who aren’t affected by the crisis. Even for the lucky ones who make it to the U.S. or another third country, it will often take years to adjust to a normal life and deal with conflict-related mental illness. That’s because after months, years, and even decades of living in chaos and fear, refugees are often stuck in “high-anxiety crisis mode,” explained Danielle Drake, community relations manager at the Cleveland Us Together office.
“If [the refugees] have nothing to do and nowhere to go, they almost create their own crisis because they don’t know how to not be in crisis mode,” Drake told Medical Daily. “I’ll have people call me and think their house is flooding, and I get there and their sink is leaking.” It takes time and resources to ease refugees into the normal hum of life in America. The most important thing, Drake said, is to make sure refugee families have a schedule. With mental health counselling, working a job, or going to school, refugees will slowly begin to recover from crisis mode. “They can adjust, and say, ‘Okay, this is my new life, I can go to work and come home and eat dinner, spend time with my family, and everything is okay,” Drake said. “There doesn’t need to be something bad that happens to me every single morning.”
Bullus says that many refugees will fill out mental health surveys when they arrive in the U.S. and say they feel no distress at all. Six months later, however, they’ll begin to exhibit signs of depression or even suicidal tendencies.
A refugee’s mental health “is that Pandora’s box that people are scared to open,” Bullus said. “The amount of families who come over with children kidnapped or husbands missing, that’s something you find out once they get here. They’re so ashamed of what happened to them, it’s going to take a while for them to open up… all their experiences are still going on, they’re still receiving threats, their families are still [in their home countries]. This is stuff that doesn’t come up with screening. The real health burden is the after-screening.”
Of course, there are often cultural challenges to mental health care. In many cultures around the globe, people who seek out mental health care may end up getting stigmatized in their community. To help refugees overcome that obstacle, local case workers get creative; sometimes, for example, they provide mental health counseling under a different name, like “community integration support groups.”
When I asked Bullus about how Ayad could find mental health assistance here, she noted that it would be more difficult for an autistic adult to be treated. “Adult refugees who resettle and claim a disability often have a difficult time having it recognized if they have no documented medical diagnoses and medical records, which many of them don’t,” Bullus explained. “Children that come over here with developmental disabilities, we immediately get them into an area hospital’s comprehensive care program... They can go to school again, they can go to summer camps… it’s really opening doors for these families who had nowhere to turn before arriving here.” For adults like Ayad, however, it’s harder because he’s gone his whole life without a diagnosis or treatment. “But between the resettlement agencies and [NFP], we try to do as much as possible to get them the care they should’ve been receiving their whole life.”

Because of this, for the Al Alawi family, overcoming “crisis mode” may be a little more difficult. Not only has Ayad lived with untreated autism his entire life, but he has also survived the trauma of moving to different countries to escape crisis. Although most of the time Ayad is “quiet and peaceful,” Khalid said, “any change is a problem for him.”
Nadia Kasvin was a Russian refugee herself, having arrived in the U.S. from the former Soviet Union in the 1990s. Her own experiences of survival are perhaps what motivate her to improve the way refugees are cared for today. One of the ways she’s doing that is by helping to spearhead a newly-formed program for survivors of torture, which helps refugees (as well as non-refugees), recover from the trauma of torture abroad.
“We see a lot of victims of gender violence and torture, and these things don’t go away by themselves,” Kasvin said. “[These issues] need a lot of effort and services, so we designed this program to provide services for social, medical, and mental health needs as well as spiritual and wellness services.” The program, which will be rolled out in Columbus, Cleveland and Toledo, aims to develop a network of partners to help build community for more sustainable services, and ultimately involve mainstream medical providers (such as Mount Carmel Hospital in Columbus) to begin offering special services to refugees suffering from the trauma of surviving torture.
“My mom and my grandmother are Holocaust survivors, and I wish someone had addressed their [emotional and mental health] issues, but they’re still not addressed,” Kasvin said. “We see the results of not addressing them. They just don’t go away; it doesn’t matter if it’s a year ago, 10 years ago, or 70 years ago. There are still huge needs that if we don’t address in a timely matter, they morph into something else, they persist, and then they come up in some different form decades later.”
Published by Medicaldaily.com



























