What to Expect When You’re Not Expecting: Freezing Egg Costs And Complications

Who are the women sitting in the waiting room with faraway eyes and brochures about egg freezing in their hands?
It’s easiest to categorize them into two strikingly different groups. One group is made up of women who face illnesses that impact fertility, including endometriosis and cancer. On the advice of their doctors and supported by families and sometimes a husband, they’re making this choice to ensure that one day, following surgery or chemo, they still have the chance to mother their own biological children. The other group includes women who hurriedly speak about jobs with late hours and business trips and little time to meet guys. Even though it seems impossible within their current, busy lives, these women hold on to the hope that some far off day in the future they will have the option to have their own children should they wish to do so.
Yet, these portraits are not necessarily distinct as many women bridge both groups. The woman who faced down, say, surgery related to endometriosis in her 20s, might be a career woman today. The single woman who took the non-stop bicoastal job she loved in her 20s discovers a lump in her breast in her 30s. Hally, 41, is one of the many who straddle both categories.
She was married and 37 when, as she puts it, “we finally froze my eggs.” Telling her story, Hally describes herself as “analytical, by nature,” more than once. A friend of a friend, we are talking on the phone. Now an internal audit manager for a bank, she previously worked for a Big Four accounting firm. Early in her career, she received a diagnosis of Crohn’s disease, a difficult, sometimes debilitating health problem (though not one that impacts fertility).
“I was focused on my career, my education, I moved to a couple of different cities, LA, Chicago — I was in San Antonio, Texas, and when I did meet somebody I fell in love with…,” she says, her voice drifting away and then returning with a sudden laugh, “Well, he’s actually 7 years younger than me. When we met I was 35 and he was 28.”
Falling in love, she immediately started thinking about getting her eggs frozen, she says, since different friends had either talked about it for themselves or undergone IVF procedures or similar fertility procedures.
“If I were still single I probably wouldn’t have done it,” she says, adding she was always someone who just lived in the present … until she fell in love and “the future question” came up and she and her future husband needed to address it. “I kind of did it because I didn’t want him to make decisions [about the future] based on my age, I wanted him to make decisions based on what was right for him,” she says.
And so the process began.
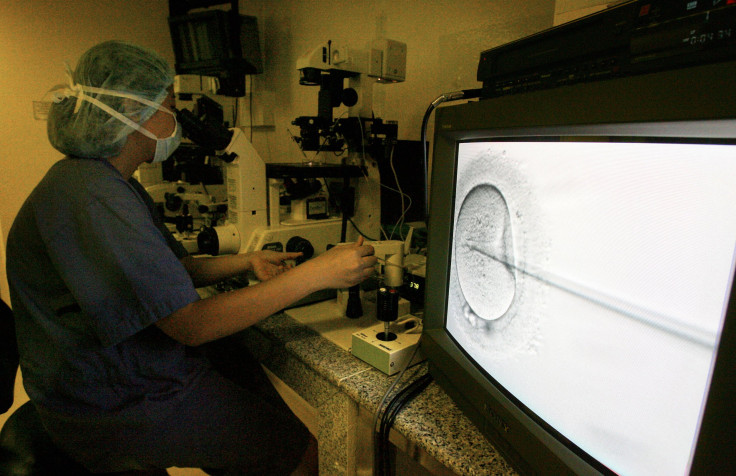
Scientists first learned how conception takes place just 173 years ago, according to PBS, when researchers discovered a sperm from the male reproductive system enters an ovum from the female reproductive system. Slightly more than a century later, in 1953, the first human birth from frozen sperm was reported followed by the first in vitro fertilization procedure, when doctors joined egg and sperm in a lab and then implanted it in a woman in 1968. Less than 20 years later, doctors reported the first human birth from a frozen embryo, which led to the first human birth from a frozen oocyte in 1986.
While “cryopreservation of sperm and embryos has been going on for decades,” says Dr. Eric Widra, medical director of Shady Grove Fertility in Washington, D.C., cryopreservation of eggs is still “a young technology and it is a finicky technology.”
“The egg is the largest, most complicated cell in humans, full of water and fussy,” says Widra, noting by comparison “sperm are simple, they’re just little DNA bots.”
There are two different techniques for freezing eggs, slow and ultra-rapid (vitrification). Both methods are intended to minimize ice crystals in the egg, which can be damaging. The slow-freeze method is older and has a lower success rate.
As Dr. Kevin Doody of the Center For Assisted Reproduction in Texas explains, egg freezing was first declared non-experimental in 2012. Although clinics had performed these procedures for some time before then, it took years to refine the techniques to the point of commercial use.
From a woman’s perspective, egg freezing is only the end of a long process that began four to six weeks earlier. First, she must take medications and injections that disable her natural hormones; next she takes hormones that stimulate her ovaries to ripen multiple eggs; and finally, her eggs are retrieved and frozen.
As Hally remembers it, you have to inject one of the drugs under your muscles: “It wasn’t so painful or uncomfortable that I wouldn’t do it again.”
Once the eggs have matured, a doctor, using ultrasound for guidance, removes them with a needle placed through her vagina. Women are sedated for this procedure, which is not considered painful. Then, the eggs are immediately frozen.
“Preparing for a colonoscopy is worse,” Hally says.
Her retrieval yielded 10 fully mature eggs and one immature egg and she froze all of them. Maturity rates after a stimulation cycle are generally 80 to 90 percent, says Widra.
“We’re only now beginning to set expectations for how many eggs are needed,” he adds, with different programs having different recommendations. “The reality is you don’t know how many are needed,” says Widra, though 20 mature eggs from a younger woman would give you about an 80 percent chance of success. For women over 35, his center recommends 30 mature eggs.
Many women say the hormones are the hardest part: PMS multiplied by 100, the proverbial emotional roller coaster. One woman writing for Brigitte Adams’s community website Eggsurance experienced “postpartum depression for about 60 days after the [egg retrieval] procedure.” By comparison, Hally did not find it difficult.
“Maybe I was a little more emotional and sensitive, but it wasn’t bad,” she says, adding with a laugh that her husband might say otherwise. Overall, the decision-making around freezing her eggs was harder, though one aspect of this was relatively easy: her choice of fertility specialist came by way of a recommendation from her physician.
“It worked fairly inexpensively,” she says, having paid “$5,000 to go through the whole cycle.”
This price tag is specific to Hally’s time, four years ago, and place, Chicago. According to Eggsurance, the cost to freeze your eggs equals those for a routine IVF — anywhere from $8,000 to $12,000, depending on the clinic. Most centers do not include the price of medications, which may set you back by $2,000 to $4,000 per cycle. Usually, though, total costs do include pre-procedure testing (blood work and ultrasounds) and monitoring.
Egg storage is a separate cost and amounts to a couple hundred dollars per year.
Most health insurance plans do not cover egg freezing. (Notable exceptions include the plans offered by tech giants Apple and Facebook, which will cover up to $20,000 worth of procedures for employees wanting to freeze their eggs.) Though you may not work at a benefits-rich company, you will want to confirm the specifics of what your own comparatively lackluster health plan does cover, since many foot the bill on blood tests, ultrasounds, or other pre-retrieval procedures.
What many women forget is that on the other side of egg freezing she will encounter an additional round of costs for egg fertilization and embryo transfer. Just like retrieval costs, these will vary depending on the clinic, some of which offer bundled rates. Total costs for both range, on average, between $6,000 and $10,000 with many clinics not including medication and work up fees.
This final half of the process is where the story becomes real: does the frozen egg turn into a baby?
From 353 frozen eggs thawed in 2012, the result was 83 live births, while 99 babies were born from 414 thaws in 2013 and 162 babies born from 718 thaws in 2014, according to numbers provided by Doody, who also serves on the executive council for the Society for Assisted Reproductive Technology (SART). Overall, this represents about a 23 percent success rate for egg freezing, though with the improved vitrification technique, scientists believe, going forward, the rate will likely be higher.
An unrelated published study finds egg survival after vitrification and warming ranged between 90 and 97 percent, fertilization rates ranged between 71 and 79 percent, implantation rates ranged between 17 and 41 percent, and clinical pregnancy rates per transfer ranged from 36 to 61 percent. (These rates may be higher because the study included frozen donor eggs, generally younger and healthier than those of women who currently choose to freeze their own eggs.)
Importantly, babies born as a result of egg freezing fall within the same odds of normal development as naturally conceived children. Asked if he worries about possible long-term issues, Doody says, “I don’t have big fears. There’s a long history of freezing sperm and a long history of freezing embryos with no apparent harm.” While egg freezing is different, there’s also a fairly established concept of egg resilience: what doesn’t destroy an egg (and this includes radiation) seems to leave it unharmed. “We do want to follow these offspring long-term,” he adds, noting they’ve done and continue to do studies looking for developmental issues.
Whether a 24 percent success rate is perceived as low risk or high, women are increasingly placing their faith in egg freezing. According to SART, nearly 500 women froze their eggs in 2009 while in 2013 nearly 5,000 did the same (these are the most recent numbers).
Widra says at his center alone they performed 250 cycles in 2014, 350 in 2015, and 450 will be done this year.
“From my perspective, this is still kind of an early adopter technology,” he says. The women who choose to freeze their eggs are comfortable with the idea, even if “it’s not quite a cell phone yet.” That said, he admits it may never be, due to financial and other barriers: “Some people feel uncomfortable about it.”
For Hally, her frozen eggs represent hope… and a few more decisions. “The question we know we have to answer sooner rather than later is, ‘Do I want to carry it?’” She believes she has until age 45 to decide since at that age she might begin to worry about her own health or the baby’s.
“Probably in the next year, I will start asking my husband how he feels about it,” she says. “We could always use [the eggs] by surrogate at any time. That’s still an option.”
Published by Medicaldaily.com



























